ADDYI Film coated tablet Ref.[10066] Active ingredients: Flibanserin
Source: FDA, National Drug Code (US) Revision Year: 2019
12.1. Mechanism of Action
The mechanism of action of ADDYI in the treatment of premenopausal women with hypoactive sexual desire disorder is not known.
12.2. Pharmacodynamics
Receptor Binding
In vitro, flibanserin demonstrated high affinity for the following serotonin (5-hydroxytryptamine or 5-HT) receptors: agonist activity at 5-HT1A and antagonist activity at 5-HT2A. Flibanserin also has moderate antagonist activities at the 5-HT2B, 5-HT2C, and dopamine D4 receptors.
Alcohol Interaction
See Clinical Trials Experience (6.1)
Cardiac Electrophysiology
The effect of ADDYI on the QT interval was evaluated in a randomized, double-blind, placebo- and active- (single dose moxifloxacin) controlled crossover study in 56 healthy men and women. Subjects in the ADDYI groups received either 50 mg twice a day (equivalent to the daily recommended dosage) or 100 mg three times a day (3 times the daily recommended dosage) administered for 5 days. The time frame for electrocardiogram (ECG) measurements covered maximum plasma concentrations of flibanserin and relevant metabolites. In this study, ADDYI did not prolong the QT interval to any clinically relevant extent. The mean increase in heart rate associated with the 100 mg three times a day dose of ADDYI compared to placebo ranged from 1.7 to 3.2 beats per minute.
12.3. Pharmacokinetics
Flibanserin showed dose-proportional pharmacokinetics for Cmax after single oral doses of 100 mg to 250 mg (the recommended and 2.5 times the recommended dosage, respectively) in healthy female subjects. Steady state was achieved after 3 days of dosing. The extent of exposure (AUC0-∞) with once-daily dosing of 100 mg of flibanserin was increased 1.4-fold as compared to a single dose.
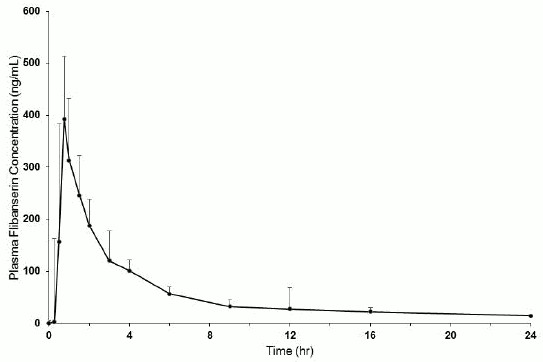
Figure 1. Mean + SD Plasma Flibanserin Concentration-Time Profiles in Healthy Female Subjects Following a Single Oral Dose of 100 mg of Flibanserin (Linear Scale):
Absorption
Following oral administration of a single 100 mg dose of flibanserin in healthy premenopausal women (N=8), mean (SD) Cmax was 419 (206) ng/mL and mean (SD) AUC0-inf was 1543 (511) ng*hr/mL. Median (range) time to reach Cmax was 0.75 (0.75 to 4.0) hours. Absolute bioavailability of flibanserin following oral dosing is 33%.
Effect of Food
Food increased the extent of absorption and slowed the rate of absorption of a 50 mg dose of flibanserin (one half the recommended dosage). Low-, moderate-, and high-fat meals increased flibanserin AUC0-inf by 1.18-, 1.43-, and 1.56-fold; increased Cmax by 1.02-, 1.13-, and 1.15-fold; and prolonged median Tmax to 1.5, 0.9, 1.8 hours from 0.8 hours under fasted conditions, respectively.
Distribution
Approximately 98% of flibanserin is bound to human serum proteins, mainly to albumin.
Elimination
Metabolism
Flibanserin is primarily metabolized by CYP3A4 and, to a lesser extent, by CYP2C19. Based on in vitro and/or in vivo data, CYP1A2, CYP2B6, CYP2C8, CYP2C9, and CYP2D6 contribute minimally to the metabolism of flibanserin. After a single oral solution dose of 50 mg 14C-radiolabeled flibanserin, 44% of the total 14C-flibanserin related radioactivity was recovered in urine, and 51% was recovered in feces. Flibanserin is extensively metabolized to at least 35 metabolites, most of them occurring in low concentrations in plasma. Two metabolites could be characterized that showed plasma concentrations similar to that achieved with flibanserin: 6,21-dihydroxy-flibanserin-6,21-disulfate and 6-hydroxy-flibanserin-6-sulfate. These two metabolites are inactive.
Excretion
Flibanserin has a mean terminal half-life of approximately 11 hours.
Specific Populations
Hepatic Impairment
Single 50 mg oral doses of flibanserin were administered to 10 patients with mild hepatic impairment (Child-Pugh score of 6 points), 4 patients with moderate hepatic impairment (Child-Pugh score of 8-9 points), and 14 healthy subjects matched by age, weight, and gender. Systemic flibanserin exposure (AUC0-inf) increased 4.5-fold in patients with mild hepatic impairment, compared to subjects with normal hepatic function, and t1/2 was longer (26 hours compared to 10 hours in matching healthy controls). Due to the small number of patients (n=4) with moderate hepatic impairment enrolled in the study, it is not possible to make conclusions about the quantitative effect of moderate hepatic impairment on flibanserin exposure. ADDYI is contraindicated in patients with hepatic impairment [see Warnings and Precautions (5.5)].
Renal Impairment
Single 50 mg oral doses of flibanserin were administered to 7 patients with mild to moderate renal impairment (GFR 30 to 80 mL/min), 9 patients with severe renal impairment (GFR <30 mL/min, not on dialysis), and 16 healthy subjects matched by age, weight, and gender. Flibanserin exposure (AUC0-inf) increased 1.1-fold in patients with mild to moderate renal impairment and 1.2-fold in patients with severe renal impairment, compared to the healthy control subjects.
Race/Ethnicity
A cross-study comparison between healthy Japanese women and Caucasian women with HSDD showed that flibanserin exposure was approximately 1.4-fold higher in Japanese women. When the mean flibanserin exposure in Japanese women was adjusted for weight, the AUCtau,ss in Japanese women was 2246 ng*hr/mL, which is comparable to 2080 ng*hr/mL in Caucasian women. The similarity in weight-adjusted AUCtau,ss suggests that weight, not race, is the factor contributing to the observed difference in flibanserin exposure between Japanese and Caucasian women.
Age
No formal study has been conducted to study the effect of age on flibanserin exposures.
Drug Interaction Studies
Drugs that Increase Flibanserin Exposure
The effects of other drugs on the pharmacokinetics of flibanserin are presented in Table 4 as change relative to flibanserin administered alone (test/reference).
Moderate CYP3A4/Moderate CYP2C9/Strong CYP2C19 Inhibitor (Fluconazole):
In a study of 15 healthy female subjects, a fluconazole 400 mg loading dose followed by 200 mg administered once daily for 5 days increased flibanserin 100 mg single dose exposure (AUC0-inf) 7-fold and Cmax 2.2-fold compared to flibanserin 100 mg alone. Three of 15 subjects (20%) experienced hypotension or syncope from concomitant use of fluconazole and flibanserin; therefore, the study was stopped early [see Warnings and Precautions (5.2), Adverse Reactions (6.1) and Drug Interactions (7)].
Strong CYP3A4 Inhibitor (Ketoconazole):
In a study of 24 healthy female subjects, ketoconazole 400 mg administered once daily for 5 days following a light breakfast increased flibanserin 50 mg single-dose exposure (AUC0-inf) 4.5-fold and Cmax 1.8-fold compared to flibanserin 50 mg alone [see Warnings and Precautions (5.2), Adverse Reactions (6.1) and Drug Interactions (7)].
Strong CYP3A4 Inhibitor (Itraconazole):
In a study of 12 healthy male and female subjects, itraconazole 200 mg administered once daily for 4 days following a loading dose of 400 mg increased flibanserin 50 mg single dose exposure (AUC0-inf) 2.6-fold and Cmax 1.7-fold when flibanserin was given 2 hours after itraconazole on Day 5, compared to exposures with flibanserin 50 mg alone. The 200 mg itraconazole dose does not maximally inhibit the CYP3A4 enzyme [see Drug Interactions (7)].
Moderate CYP3A4 Inhibitor (Grapefruit Juice):
In a study of 26 healthy female subjects, grapefruit juice (240 mL) increased flibanserin 100 mg single dose exposure (AUC0-inf) by 1.4-fold and Cmax 1.1-fold compared to flibanserin 100 mg alone [see Warnings and Precautions (5.2), Adverse Reactions (6.1) and Drug Interactions (7)].
Weak CYP3A4 Inhibitor (Oral Contraceptives):
In a meta-analysis of 17 oral contraceptive users and 91 non-users in Phase 1 studies, the oral contraceptive users had a 1.4-fold higher flibanserin AUC and 1.3‑fold higher Cmax compared to the non-users [see Adverse Reactions (6.1) and Drug Interactions (7)].
Strong CYP2D6 Inhibitor (Paroxetine):
Paroxetine is a strong CYP2D6 inhibitor. In a study of 19 healthy male and female subjects, flibanserin exposure decreased by approximately 4% when flibanserin 50 mg twice daily was given with paroxetine compared to flibanserin alone. Paroxetine was dosed at 20 mg once daily for 3 days followed by 40 mg once daily for 7 days.
Drugs that Decrease Flibanserin Exposure
Strong CYP3A4 Inducer (Rifampin):
In a study of 24 healthy female subjects, rifampin 600 mg given once daily for 7 days prior to administration of 100 mg flibanserin significantly decreased flibanserin exposure by 95% [see Drug Interactions (7)].
Moderate CYP3A4 Inducer (Etravirine):
Steady state etravirine, a moderate CYP3A4 inducer, decreased flibanserin exposures by approximately 21% [see Drug Interactions (7)].
Table 4. Drugs That Increase Flibanserin Exposure:
| Coadministered Drug(s) and Dose(s) | Dose of ADDYI | n | Geometric Mean Ratio (90% Confidence Interval) of Pharmacokinetic Parameters of Flibanserin with/without Coadministered Drug No Effect=1.00 | |
|---|---|---|---|---|
| Cmax | AUC0-inf | |||
| Fluconazole 200 mg | 100 mg | 15 | 2.2 (1.8–2.8) | 7.0 (6.0–8.2) |
| Ketoconazole 400 mg | 50 mg | 24 | 1.8 (1.7–2.1) | 4.5 (4.0–5.1) |
| Itraconazole 200 mg* | 50 mg | 12 | 1.7 (1.4–2.0) | 2.6 (2.1–3.0) |
| Oral Contraceptives | 50 mg | 39 | 1.3 (1.1–1.6) | 1.4 (1.2–1.7) |
| Paroxetine 40 mg | 50 mg twice daily | 19 | 1.0 (0.9–1.2) | 1.0 (0.9–1.0) |
* itraconazole dose was not optimal for maximal inhibition of CYP3A4 enzyme.
Effects of Flibanserin on Other Drugs
The effects of flibanserin on the pharmacokinetics of other drugs are presented in Table 5 as change relative to the other drug administered alone (test/reference).
Digoxin and P-glycoprotein Substrates:
A single center, open-label, randomized, two-way crossover study in 24 healthy men and women evaluated the effect of flibanserin on the pharmacokinetics of digoxin. Flibanserin 100 mg was administered once daily over 5 days followed by a single dose of 0.5 mg digoxin, a P-gp substrate. Flibanserin increased digoxin AUC0-inf by 2.0-fold and Cmax by 1.5-fold, compared to digoxin alone [see Drug Interactions (7)].
Drugs Metabolized by CYP3A4 (Simvastatin):
An open-label, randomized, crossover study in 12 healthy men and women evaluated the effect of flibanserin 50 mg twice daily for 4 days on the pharmacokinetics of simvastatin 40 mg once daily. Flibanserin increased the AUC0-inf of simvastatin, a substrate of CYP3A4, 1.3‑fold and Cmax by 1.2-fold. Flibanserin co-administered with simvastatin increased simvastatin acid AUC0-inf by 1.5-fold and Cmax by 1.4-fold.
Oral Contraceptives:
A study in 24 healthy women evaluated the effect of 100 mg flibanserin once daily for 2 weeks on the pharmacokinetics of a single-dose of ethinyl estradiol (EE) 30 mcg/levonorgestrel (LNG) 150 mcg. Flibanserin increased the EE AUC0-inf by 1.09-fold and the EE Cmax by 1.1-fold. Flibanserin decreased the LNG AUC0-inf by 1.06-fold and did not change the LNG Cmax [see Adverse Events (6.1), Drug Interactions (7)].
Drugs Metabolized by CYP2B6 (Bupropion):
An open-label, randomized, two-period crossover study in 28 healthy women evaluated the effect of flibanserin on the pharmacokinetics of bupropion. Flibanserin 50 mg twice daily was administered for 2 days followed by 100 mg once daily for 13 days. Bupropion 150 mg twice daily was given for 8 days beginning on Day 6 of flibanserin treatment. Flibanserin did not change bupropion AUCt,ss (1.0-fold change) and Cmax (1.0-fold change) but hydroxybupropion AUCt,ss decreased by 9% and Cmax by 11%.
Table 5. Effects of Flibanserin on Exposure of Other Drugs:
| Coadministered Drug(s) and Dose(s) | Dose of ADDYI | n | Geometric Mean Ratio (90% Confidence Interval) of Pharmacokinetic Parameters of Coadministered Drug with/without Flibanserin No Effect=1.00 | |
|---|---|---|---|---|
| Cmax | AUC0-inf | |||
| Simvastatin 40 mg | 50 mg twice daily | 12 | 1.7 (1.4–2.0) | 2.6 (2.1–3.1) |
| Digoxin 0.5 mg | 100 mg | 24 | 1.5 (1.3–1.6) | 2.0 (1.5–2.5) |
| Ethinyl estradiol 30 mcg/ Levonorgestrel 150 mcg | 100 mg | 24 | 1.1 (1.0–1.1) 1.0 (0.9–1.0) | 1.1 (1.0–1.2) 1.0 (0.9–1.1) |
| Bupropion 150 mg | 100 mg | 28 | 1.0 (0.9–1.1) | 1.0 (1.0–1.1) |
12.5. Pharmacogenomics
Patients who are poor metabolizers of CYP2D6, CYP2C9 or CYP2C19 are deficient in CYP2D6, CYP2C9 or CYP2C19 enzyme activity, respectively. Extensive metabolizers have normal functioning CYP enzymes.
CYP2C19 Poor Metabolizers
A study comparing flibanserin exposure in CYP2C19 poor metabolizers to CYP2C19 extensive metabolizers was conducted in lieu of a drug interaction study with ADDYI and a strong CYP2C19 inhibitor. In 9 women who were poor metabolizers of CYP2C19, Cmax and AUC0-inf of flibanserin 100 mg once daily increased 1.5-fold (1.1-2.1) and 1.3-fold (0.9-2.1), compared to exposures among 8 extensive metabolizers of CYP2C19. Flibanserin half-life was increased from 11.1 hours in the extensive metabolizers of CYP2C19 to 13.5 hours in the poor metabolizers of CYP2C19 [see Adverse Reactions (6.1) and Use in Specific Populations (8.7)].
The frequencies of poor metabolizers of CYP2C19 are approximately 2–5% among Caucasians and Africans and approximately 2–15% among Asians.
CYP2D6 Poor Metabolizers
A study comparing flibanserin exposure in CYP2D6 poor metabolizers to CYP2D6 extensive metabolizers was conducted in addition to a drug interaction study with paroxetine, a strong CYP2D6 inhibitor. In 12 poor metabolizers of CYP2D6, steady state Cmax and AUC of flibanserin 50 mg twice daily was decreased by 4% and increased by 18%, respectively, compared to exposures among 19 extensive metabolizers, intermediate metabolizers and ultra rapid metabolizers of CYP2D6.
CYP2C9 Poor Metabolizers
A study comparing flibanserin exposure in CYP2C9 poor metabolizers to CYP2C9 extensive metabolizers was conducted in lieu of a drug interaction study with ADDYI and a strong CYP2C9 inhibitor. In 8 women who were poor metabolizers of CYP2C9, Cmax and AUC0-inf of flibanserin 100 mg once daily decreased 23% and 18%, compared to exposures among 8 extensive metabolizers of CYP2C9.
13.1. Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenesis
A two-year carcinogenicity study was conducted in CD-1 mice with dietary administration of 0, 10, 80, 200 and 1000/1200 mg/kg/day of flibanserin. Statistically significant increases in combined mammary tumors (adenoacanthomas and adenocarcinomas) were observed in female mice administered flibanserin at doses of 200 and 1200 mg/kg/day (exposures, based on AUC, were 3 and 10 times the clinical exposures at the recommended clinical dose). No increases in mammary tumors were observed in male mice. Statistically significant increases were also seen for combined hepatocellular adenomas/carcinomas in female mice treated with flibanserin 1200 mg/kg/day and for hepatocellular carcinomas in male mice treated with flibanserin 1000 mg/kg/day (exposures, based on AUC, were 8 times the clinical exposure at the recommended clinical dose).
There were no significant increases in tumor incidence in a two year carcinogenicity study conducted in Wistar rats with dietary administration of 0, 10, 30 and 100 mg/kg/day flibanserin (up to 5-8 times human exposure at the recommended clinical dose).
Mutagenesis
Flibanserin was negative for mutagenesis in vitro in Salmonella typhimurium (Ames test) and in Chinese hamster ovary cells. Flibanserin was positive for chromosomal aberrations in cultured human lymphocytes but negative for chromosomal aberrations in vivo in the rat bone marrow micronucleus assay and negative for DNA damage in rat liver in the Comet assay.
Impairment of Fertility
Female and male rats were administered flibanserin 14 and 28 days before mating, respectively, to assess for potential effects on fertility and early reproductive performance. Flibanserin slightly increased the duration of the estrus cycle but had no adverse effects on fertility or early embryonic development at doses up to 200 mg/kg/day (~20 times human exposure at the recommended clinical dose).
14. Clinical Studies
14.1 Trials in Premenopausal HSDD Patients
The efficacy of ADDYI for the treatment of HSDD in premenopausal women was established in three 24-week, randomized, double-blind, placebo-controlled trials (Studies 1, 2, and 3). The three trials included premenopausal women with acquired, generalized HSDD of at least 6 months duration. In the clinical trials, acquired HSDD was defined as HSDD that developed in patients who previously had no problems with sexual desire. Generalized HSDD was defined as HSDD that was not limited to certain types of stimulation, situations or partners. The patients were treated with ADDYI 100 mg once daily at bedtime (n=1187) or placebo (n=1188). Most of the trial participants were Caucasian (88.6%); the remainder were Black (9.6%) and Asian (1.5%). The mean age of study participants was 36 years old (range 19 to 55 years old); the mean duration in the monogamous, heterosexual relationship was 11 years, and the mean duration of HSDD was approximately 5 years. The completion rate across these three trials was 69% and 78% for the ADDYI and placebo groups, respectively.
These trials each had two co-primary efficacy endpoints, one for satisfying sexual events (SSEs) and the other for sexual desire:
- The change from baseline to Week 24 in the number of monthly SSEs (i.e., sexual intercourse, oral sex, masturbation, or genital stimulation by the partner). The SSEs were based on patient responses to the following questions: "Did you have a sexual event?" and "Was the sex satisfying for you?"
- Studies 1 and 2 had a different sexual desire endpoint than Study 3:
- In Studies 1 and 2, the sexual desire co-primary endpoint was the change from baseline to Week 24 in the calculated monthly sexual desire score and was based on patient responses to the question: "Indicate your most intense level of sexual desire." Every day, patients rated their sexual desire level from 0 (no desire) to 3 (strong desire) and recorded their response in an electronic Diary (eDiary). These responses were summed over a 28-day period to yield the calculated monthly sexual desire score, which ranged from 0 to 84.
- In Study 3, the desire domain of the Female Sexual Function Index (FSFI Desire) was the sexual desire co-primary endpoint. The desire domain of the FSFI has two questions. The first question asks patients "Over the past 4 weeks, how often did you feel sexual desire or interest?", with responses ranging from 1 (almost never or never) to 5 (almost always or always). The second question asks patients "Over the past 4 weeks, how would you rate your level (degree) of sexual desire or interest?", with responses ranging from 1 (very low or none at all) to 5 (very high). The FSFI Desire score was calculated by adding the patient's responses to these two questions then multiplying that sum by 0.6. The FSFI Desire domain score ranged from 1.2 to 6.
The desire domain of the Female Sexual Function Index (FSFI Desire) was also used as a secondary endpoint in Studies 1 and 2.
The three trials had a secondary endpoint that measured bother (a component of distress) related to sexual desire using Question 13 of the Female Sexual Distress Scale-Revised (FSDS-R). This question asks "How often did you feel: Bothered by low sexual desire?" Patients assessed their sexual distress over a 7-day recall period and responded on a scale of 0 (never) to 4 (always).
The efficacy results from Studies 1, 2, and 3 are summarized in Table 6. In all three trials, ADDYI resulted in statistically significant improvement compared to placebo in the change from baseline in monthly SSEs at Week 24. In Study 1 and 2, there were no statistically significant differences between ADDYI and placebo for the eDiary sexual desire endpoint (change in baseline to Week 24). In contrast, in Study 3 there was statistically significant improvement in the change from baseline to Week 24 in sexual desire (using the FSFI Desire Domain) with ADDYI compared to placebo. The FSFI Desire Domain findings were consistent across all three trials as were the findings for the secondary endpoint that assessed distress using Question 13 of the FSDS-R.
Table 6. Efficacy Results in Premenopausal HSDD Patients in Studies 1, 2, and 3:
| Study 1 | Study 21 | Study 3 | ||||
|---|---|---|---|---|---|---|
| ADDYI | Placebo | ADDYI | Placebo | ADDYI | Placebo | |
| Full Analysis Set | n=280 | n=290 | n=365 | n=372 | n=532 | n=536 |
| Number of satisfying sexual events (per 28 days) | ||||||
| Baseline (Mean) | 3.0 | 2.7 | 2.6 | 2.7 | 2.5 | 2.7 |
| Change from baseline (Mean) | 1.6 | 0.8 | 1.8 | 1.1 | 2.5 | 1.5 |
| Treatment diff. (95% CI) | 0.9 (0.3, 1.4) | 0.6 (-0.03, 1.2) | 1.0 (0.4, 1.5) | |||
| Change from baseline (Median) | 1.0 | 0.0 | 1.0 | 0.5 | 1.0 | 0.5 |
| Median treatment difference | 1.0 | 0.5 | 0.5 | |||
| p-value vs placebo | p<0.01 | p<0.01 | p<0.0001 | |||
| e-Diary Desire | ||||||
| Baseline (Mean) | 12.9 | 11.8 | 12.1 | 10.2 | Not Used | Not Used |
| Change from baseline at Week 24 (Mean) | 9.1 | 6.9 | 8.3 | 6.7 | ||
| Treatment diff. (95% CI) | 2.3 (-0.1, 4.7) | 1.7 (-0.5, 4.0) | ||||
| p-value vs placebo | NS | NS | ||||
| FSFI Desire | ||||||
| Baseline (Mean) | 1.9 | 1.9 | 1.8 | 1.8 | 1.9 | 1.9 |
| Change from baseline at Week 24 (Mean) | 0.9 | 0.5 | 0.9 | 0.5 | 1.0 | 0.7 |
| Treatment diff. (95% CI) | 0.4 (0.2, 0.5) | 0.3 (0.2, 0.5) | 0.3 (0.2, 0.4) | |||
| p-value vs placebo | N/A2 | N/A2 | p<0.0001 | |||
| FSDS-R Question 133 | ||||||
| Baseline (Mean) | 3.2 | 3.2 | 3.2 | 3.2 | 3.4 | 3.4 |
| Change from baseline at Week 24 (Mean) | -0.8 | -0.5 | -0.8 | -0.5 | -1.0 | -0.7 |
| Treatment diff. (95% CI) | -0.4 (-0.5, -0.2) | -0.3 (-0.4, -0.1) | -0.3 (-0.4, -0.1) | |||
| p-value vs placebo | N/A2 | N/A 2 | p=0.0001 | |||
CI = Confidence Interval; NS = not statistically significant; N/A=not applicable
Shaded cells show the results for the co-primary efficacy endpoints for each trial.
e-Diary desire was evaluated as a co-primary endpoint in Studies 1 and 2; FSFI desire was evaluated as a co-primary endpoint in Study 3.
The efficacy results are based on the full analysis set comprised of all randomized patients who took at least one dose of study medication and had at least one on-treatment efficacy assessment. Missing values were imputed using last-observation-carried-forward.
The unadjusted means are presented for the baseline values.
For satisfying sexual events, p-values are based on the Wilcoxon rank sum test stratified by pooled center. Median change from baseline is shown because the data are not normally distributed.
For FSFI-desire, e-Diary desire, and FSDS-R Question 13, reported p-values are based on an ANCOVA model using baseline as a covariate with treatment and pooled center as main effect terms. For the change from baseline, the adjusted least squares mean (standard error) are presented.
1 Excludes subjects from two study sites that had data integrity issues
2 p-value not reported for secondary endpoints because the trial failed on the eDiary Desire co-primary efficacy endpoint
3 A decrease in score represents improvement
Exploratory analyses were conducted to assess whether the treatment effects varied depending on baseline number of SSEs, FSFI desire score, and FSDS-R Question 13 distress score. No notable differences were identified among these subgroups.
Supportive analyses were conducted to help interpret the clinical meaningfulness of the observed treatment effects. These analyses defined responders for each efficacy endpoint by anchoring change from baseline to end of treatment with the Patient's Global Impression of Improvement (PGI‑I). The first analysis considered responders to be those who reported being "much improved" or "very much improved." In this analysis, the absolute difference in the percentage of responders with ADDYI and the percentage of responders with placebo across the three trials was 8-9% for SSEs (29-39% for ADDYI; 21-31% for placebo), 10-13% for FSFI desire domain (43-48% for ADDYI; 31-38% for placebo), and 7-13% for FSDS-R Question 13 (21-34% for ADDYI; 14-25% for placebo). The second analysis considered responders to be those who reported being at least minimally improved. The absolute difference in the percentage of responders with ADDYI and the percentage of responders with placebo across the three trials was 10-15% for SSEs (44-48% for ADDYI; 33-36% for placebo), 12-13% for FSFI desire domain (43-51% for ADDYI; 31-39% for placebo), and 9-12% for FSDS-R Question 13 (50-60% for ADDYI; 41-48% for placebo).
14.2 Effects on Driving
In a randomized, placebo-controlled, 4-way crossover study in 83 healthy premenopausal female subjects, no adverse effect was detected on measures of driving performance itself or psychomotor performance thought to be important for driving performance when assessed 9 hours following single and multiple doses of ADDYI 100 mg once daily at bedtime or single doses of ADDYI 200 mg at bedtime (two times the maximum recommended dosage) [see Warnings and Precautions (5.3)].
© All content on this website, including data entry, data processing, decision support tools, "RxReasoner" logo and graphics, is the intellectual property of RxReasoner and is protected by copyright laws. Unauthorized reproduction or distribution of any part of this content without explicit written permission from RxReasoner is strictly prohibited. Any third-party content used on this site is acknowledged and utilized under fair use principles.