CRESEMBA Hard capsule Ref.[9619] Active ingredients: Isavuconazole
Source: European Medicines Agency (EU) Revision Year: 2024 Publisher: Basilea Pharmaceutica Deutschland GmbH, Marie-Curie-Strasse 8, 79539, Lörrach, Germany
Contraindications
Hypersensitivity to the active substance or to any of the excipients listed in section 6.1.
Co-administration with ketoconazole (see section 4.5).
Co-administration with high-dose ritonavir (>200 mg every 12 hours) (see section 4.5).
Co-administration with strong CYP3A4/5 inducers such as rifampicin, rifabutin, carbamazepine, long-acting barbiturates (e.g. phenobarbital), phenytoin and St. John’s wort or with moderate CYP3A4/5 inducers such as efavirenz, nafcillin and etravirine (see section 4.5).
Patients with familial short QT syndrome (see section 4.4).
Special warnings and precautions for use
Hypersensitivity
Hypersensitivity to isavuconazole may result in adverse reactions that include: anaphylactic reaction, hypotension, respiratory failure, dyspnoea, drug eruption, pruritus, and rash (see section 4.8). In case of anaphylactic reaction, isavuconazole should be discontinued immediately and appropriate medical treatment should be initiated.
Caution should be used in prescribing isavuconazole to patients with hypersensitivity to other azole antifungal agents.
Severe cutaneous adverse reactions
Severe cutaneous adverse reactions, such as Stevens-Johnson syndrome, have been reported during treatment with azole antifungal agents. If a patient develops a severe cutaneous adverse reaction, CRESEMBA should be discontinued.
Cardiovascular
QT shortening
Isavuconazole is contraindicated in patients with familial short QT syndrome (see section 4.3). In a QT study in healthy human subjects, isavuconazole shortened the QTc interval in a concentration-related manner. For the 200 mg dosing regimen, the least squares mean (LSM) difference from placebo was 13.1 ms at 2 hours post dose [90% CI: 17.1, 9.1 ms]. Increasing the dose to 600 mg resulted in an LSM difference from placebo of 24.6 ms at 2 hours post dose [90% CI: 28.7, 20.4 ms].
Caution is warranted when prescribing isavuconazole to patients taking other medicinal products known to decrease the QT interval, such as rufinamide.
Elevated liver transaminases or hepatitis
Elevated liver transaminases have been reported in clinical studies (see section 4.8). The elevations in liver transaminases rarely required discontinuation of isavuconazole. Monitoring of hepatic enzymes should be considered, as clinically indicated. Hepatitis has been reported with azole antifungal agents including isavuconazole.
Severe hepatic impairment
Isavuconazole has not been studied in patients with severe hepatic impairment (Child-Pugh Class C). Use in these patients is not recommended unless the potential benefit is considered to outweigh the 5 risks. These patients should be carefully monitored for potential drug toxicity (see sections 4.2, 4.8 and 5.2).
Paediatric patients
Isavuconazole has not been studied in paediatric patients with renal or hepatic impairment.
Paediatric patients from 6 years to less than 18 years of age and with a bodyweight at least 32 kg may receive CRESEMBA 100 mg capsules. However, the use of CRESEMBA 100 mg capsules has not been studied in paediatric patients.
Concomitant use with other medicinal products
CYP3A4/5 inhibitors
Ketoconazole is contraindicated (see section 4.3). For the strong CYP3A4 inhibitor lopinavir/ritonavir, a two-fold increase in isavuconazole exposure was observed. For other strong CYP3A4/5 inhibitors, a less pronounced effect can be expected. No dose adjustment of isavuconazole is necessary when co- administered with strong CYP3A4/5 inhibitors, however caution is advised as adverse drug reactions may increase (see section 4.5).
CYP3A4/5 inducers
Co-administration with mild CYP3A4/5 inducers such as aprepitant, prednisone, and pioglitazone, may result in mild to moderate decreases of isavuconazole plasma levels; co-administration with mild CYP3A4/5 inducers should be avoided unless the potential benefit is considered to outweigh the risk (see section 4.5).
CYP3A4/5 substrates including immunosuppressants
Isavuconazole can be considered a moderate inhibitor of CYP3A4/5, and systemic exposure to medicinal products metabolised by CYP3A4 may be increased when co-administered with isavuconazole. Concomitant use of isavuconazole with CYP3A4 substrates such as the immunosuppressants tacrolimus, sirolimus or ciclosporin may increase the systemic exposure to these medicinal products. Appropriate therapeutic drug monitoring and dose adjustment may be necessary during co-administration (see section 4.5).
CYP2B6 substrates
Isavuconazole is an inducer of CYP2B6. Systemic exposure to medicinal products metabolised by CYP2B6 may be decreased when co-administered with isavuconazole. Therefore, caution is advised when CYP2B6 substrates, especially medicinal products with a narrow therapeutic index such as cyclophosphamide, are co-administered with isavuconazole. The use of the CYP2B6 substrate efavirenz with isavuconazole is contraindicated because efavirenz is a moderate inducer of CYP3A4/5 (see section 4.3).
P-gp substrates
Isavuconazole may increase the exposure of medicinal products that are P-gp substrates. Dose adjustment of medicinal products that are P-gp substrates, especially medicinal products with a narrow therapeutic index such as digoxin, colchicine and dabigatran etexilate, may be needed when concomitantly administered with isavuconazole (see section 4.5).
Limitations of the clinical data
The clinical data for isavuconazole in the treatment of mucormycosis are limited to one prospective non-controlled clinical study in 37 adult patients with proven or probable mucormycosis who received isavuconazole for primary treatment, or because other antifungal treatments (predominantly amphotericin B) were inappropriate.
For individual Mucorales species, the clinical efficacy data are very limited, often to one or two patients (see section 5.1). Susceptibility data were available in only a small subset of cases. These data indicate that concentrations of isavuconazole required for inhibition in vitro are very variable between genera/species within the order of Mucorales, and generally higher than concentrations required to inhibit Aspergillus species. It should be noted that there was no dose-finding study in mucormycosis, and patients were administered the same dose of isavuconazole as was used for the treatment of invasive aspergillosis.
Interaction with other medicinal products and other forms of interaction
Potential of medicinal products to affect the pharmacokinetics of isavuconazole
Isavuconazole is a substrate of CYP3A4 and CYP3A5 (see section 5.2). Co-administration of medicinal products which are inhibitors of CYP3A4 and/or CYP3A5 may increase the plasma concentrations of isavuconazole. Co-administration of medicinal products which are inducers of CYP3A4 and/or CYP3A5 may decrease the plasma concentrations of isavuconazole.
Medicinal products that inhibit CYP3A4/5
Co-administration of isavuconazole with the strong CYP3A4/5 inhibitor ketoconazole is contraindicated, since this medicinal product can significantly increase plasma concentrations of isavuconazole (see sections 4.3 and 4.5).
For the strong CYP3A4 inhibitor lopinavir/ritonavir, a two-fold increase in isavuconazole exposure was observed. For other strong CYP3A4 inhibitors, such as clarithromycin, indinavir and saquinavir, a less pronounced effect can be expected, based on their relative potency. No dose adjustment of isavuconazole is necessary when co-administered with strong CYP3A4/5 inhibitors, however caution is advised as adverse drug reactions may increase (see section 4.4).
No dose adjustment is warranted for moderate to mild CYP3A4/5 inhibitors.
Medicinal products that induce CYP3A4/5
Co-administration of isavuconazole with potent CYP3A4/5 inducers such as rifampicin, rifabutin, carbamazepine, long-acting barbiturates (e.g., phenobarbital), phenytoin and St. John’s wort, or with moderate CYP3A4/5 inducers such as efavirenz, nafcillin and etravirine, is contraindicated, since these medicinal products can significantly decrease plasma concentrations of isavuconazole (see section 4.3).
Co-administration with mild CYP3A4/5 inducers such as aprepitant, prednisone and pioglitazone, may result in mild to moderate decreases of isavuconazole plasma levels; co-administration with mild CYP3A4/5 inducers should be avoided unless the potential benefit is considered to outweigh the risk (see section 4.4).
Co-administration with high-dose ritonavir (>200 mg twice daily) is contraindicated, as at high doses ritonavir may induce CYP3A4/5 and decrease isavuconazole plasma concentrations (see section 4.3).
Potential for isavuconazole to affect exposures of other medicines
Medicinal products metabolised by CYP3A4/5
Isavuconazole is a moderate inhibitor of CYP3A4/5; co-administration of isavuconazole with medicinal products which are substrates of CYP3A4/5 may result in increased plasma concentrations of these medicinal products.
Medicinal products metabolised by CYP2B6
Isavuconazole is a mild CYP2B6 inducer; co-administration of isavuconazole may result in decreased plasma concentrations of CYP2B6 substrates.
Medicinal products transported by P-gp in the intestine
Isavuconazole is a mild inhibitor of P-glycoprotein (P-gp); co-administration with isavuconazole may result in increased plasma concentrations of P-gp substrates.
Medicinal products transported by BCRP
Isavuconazole is an inhibitor in vitro of BCRP, and plasma concentrations of substrates of BCRP may therefore be increased. Caution is advised when isavuconazole is given concomitantly with substrates of BCRP.
Medicinal products renally excreted via transport proteins
Isavuconazole is a mild inhibitor of the organic cation transporter 2 (OCT2). Co-administration of isavuconazole with medicinal products which are substrates of OCT2 may result in increased plasma concentrations of these medicinal products.
Uridine diphosphate-glucuronosyltransferases (UGT) substrates
Isavuconazole is a mild inhibitor of UGT. Co-administration of isavuconazole with medicinal products which are substrates of UGT may result in mildly increased plasma concentrations of these medicinal products.
Interaction table
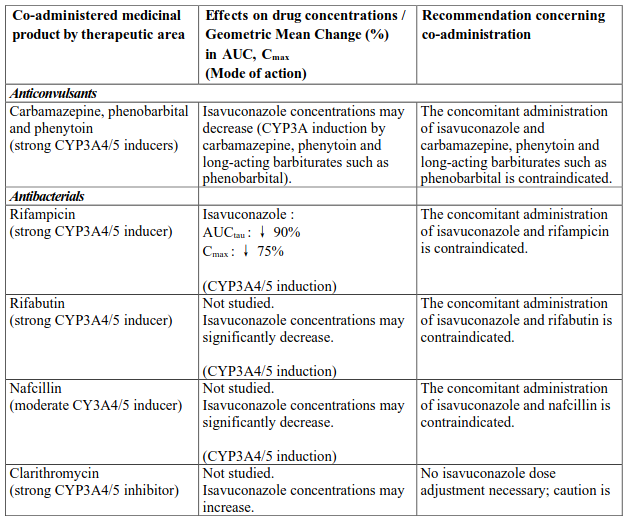
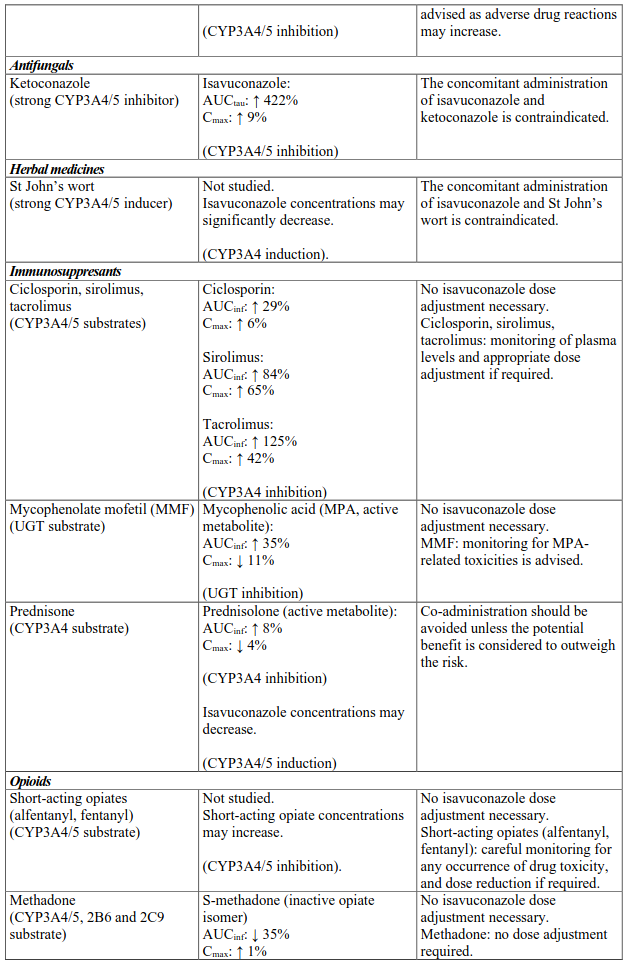
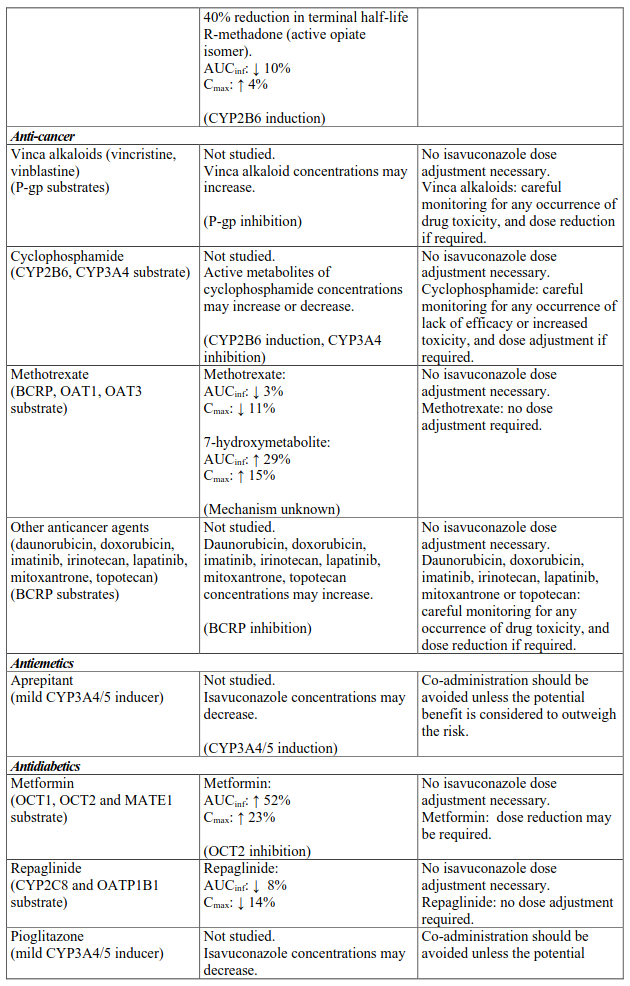
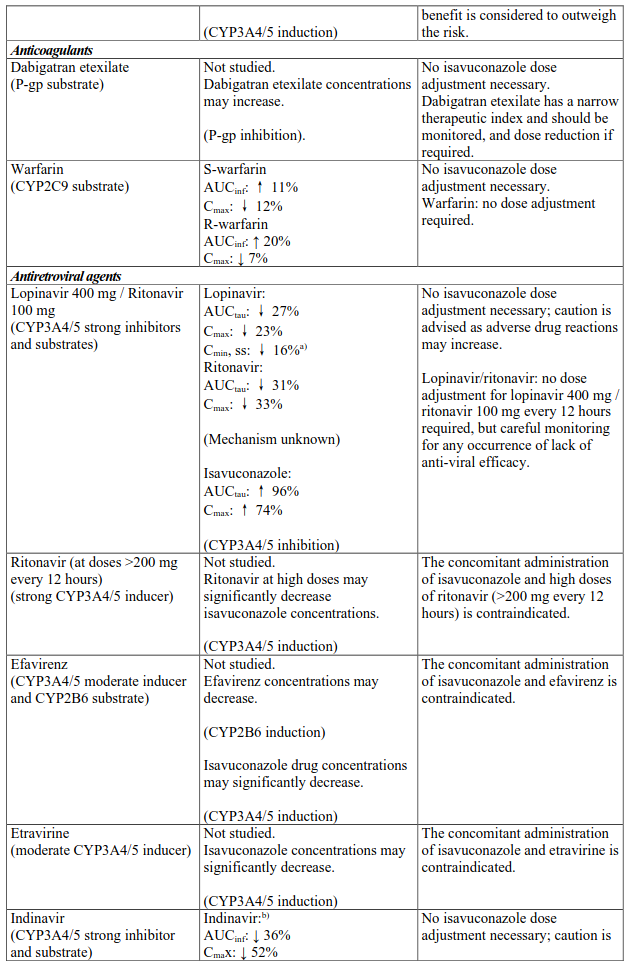
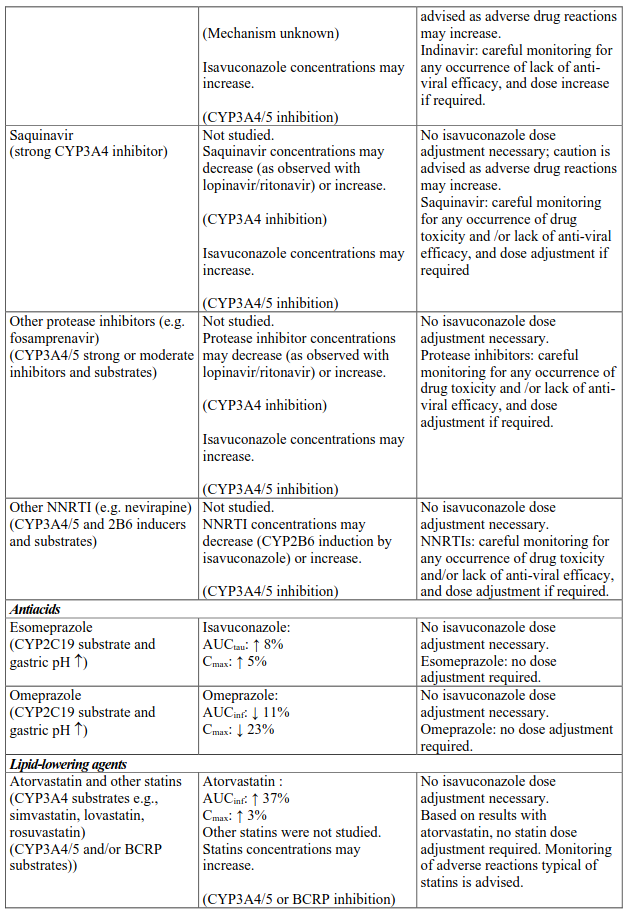
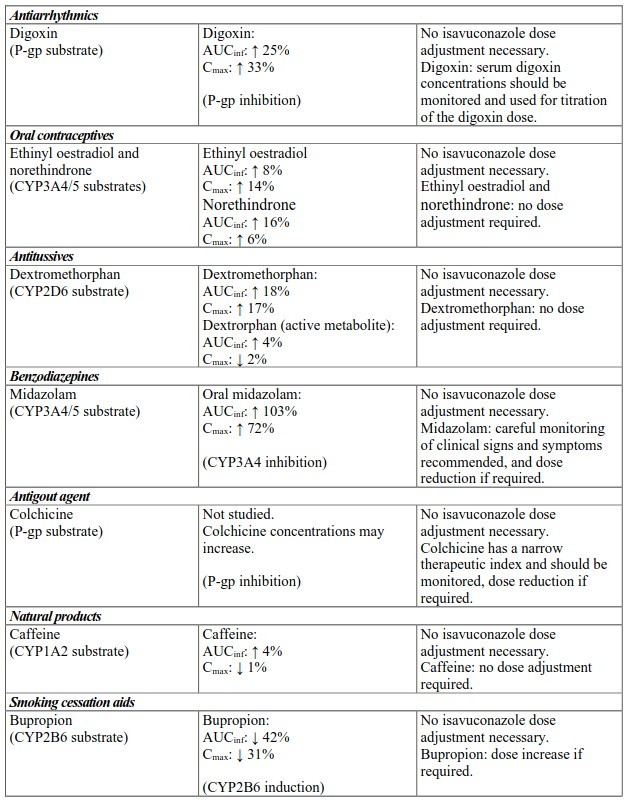
Interactions between isavuconazole and co-administered medicinal products are listed in Table 3 (increase is indicated as “↑”, decrease as “↓”), ordered by therapeutic class. Unless otherwise stated, studies detailed in Table 2 have been performed in adults with the recommended dose of isavuconazole.
Table 3. Interactions:
NNRTI, non-nucleoside reverse-transcriptase inhibitor; P-gp, P-glycoprotein.
a % decrease of the mean trough level values
b Indinavir was only studied after a single dose of 400 mg isavuconazole.
AUCinf = area under the plasma concentration-time profiles extrapolated to infinity; AUCtau = area under the plasma concentration-time profiles during the 24 h interval at steady state; Cmax = peak plasma concentration; Cmin,ss = trough levels at steady state.
Fertility, pregnancy and lactation
Pregnancy
There are no data from the use of CRESEMBA in pregnant women. Studies in animals have shown reproductive toxicity (see section 5.3). The potential risk for humans is unknown.
CRESEMBA must not be used during pregnancy except in patients with severe or potentially life-threatening fungal infections, in whom isavuconazole may be used if the anticipated benefits outweigh the possible risks to the foetus.
Women of child-bearing potential
CRESEMBA is not recommended for women of childbearing potential who are not using contraception.
Breast-feeding
Available pharmacodynamic/toxicological data in animals have shown excretion of isavuconazole/metabolites in milk (see section 5.3).
A risk to newborns and infants cannot be excluded.
Breast-feeding should be discontinued during treatment with CRESEMBA.
Fertility
There are no data on the effect of isavuconazole on human fertility. Studies in animals did not show impairment of fertility in male or female rats (see section 5.3).
Effects on ability to drive and use machines
Isavuconazole has a moderate potential to influence the ability to drive and use machines. Patients should avoid driving or operating machinery if symptoms of confusional state, somnolence, syncope, and/or dizziness are experienced.
Undesirable effects
Summary of the safety profile
The most common treatment-related adverse reactions in adults were elevated liver chemistry tests (7.9%), nausea (7.4%), vomiting (5.5%), dyspnoea (3.2%), abdominal pain (2.7%), diarrhoea (2.7%), injection site reaction (2.2%), headache (2.0%), hypokalaemia (1.7%) and rash (1.7%).
The adverse reactions which most often led to permanent discontinuation of isavuconazole treatment in adults were confusional state (0.7%), acute renal failure (0.7%), increased blood bilirubin (0.5%), convulsion (0.5%), dyspnoea (0.5%), epilepsy (0.5%), respiratory failure (0.5%) and vomiting (0.5%).
Tabulated list of adverse reactions
Table 4 presents adverse reactions with isavuconazole in the treatment of invasive fungal infections in adults, by System Organ Class and frequency.
The frequency of adverse reactions is defined as follows: very common (≥1/10); common (≥1/100 to <1/10); and uncommon (≥1/1,000 to <1/100); not known (frequency cannot be estimated from available data).
Within each frequency grouping, adverse reactions are presented in order of decreasing seriousness.
Table 4. Summary of adverse reactions by MedDRA System Organ Class and frequency:
| System Organ Class | Adverse Drug Reactions |
|---|---|
| Blood and lymphatic system disorders | |
| Uncommon | Neutropenia; Thrombocytopenia^; Pancytopenia; Leukopenia^; Anaemia^ |
| Immune system disorders | |
| Uncommon | Hypersensitivity^ |
| Not known | Anaphylactic reaction* |
| Metabolism and nutrition disorders | |
| Common | Hypokalaemia; Decreased appetite |
| Uncommon | Hypomagnesaemia; Hypoglycaemia; Hypoalbuminaemia; Malnutrition^ |
| Psychiatric disorders | |
| Common | Delirium^# |
| Uncommon | Depression; Insomnia^ |
| Nervous system disorders | |
| Common | Headache; Somnolence |
| Uncommon | Convulsion^; Syncope; Dizziness; Paraesthesia^; Encephalopathy; Presyncope; Neuropathy peripheral; Dysgeusia |
| Ear and labyrinth disorders | |
| Uncommon | Vertigo |
| Cardiac disorders | |
| Uncommon | Atrial fibrillation; Tachycardia; Bradycardia^; Palpitations; Atrial flutter; Electrocardiogram QT shortened; Supraventricular tachycardia; Ventricular extrasystoles; Supraventricular extrasystoles |
| Vascular disorders | |
| Common | Thrombophlebitis^ |
| Uncommon | Circulatory collapse; Hypotension |
| Respiratory, thoracic and mediastinal disorders | |
| Common | Dyspnoea^; Acute respiratory failure^ |
| Uncommon | Bronchospasm; Tachypnoea; Haemoptysis; Epistaxis |
| Gastrointestinal disorders | |
| Common | Vomiting; Diarrhoea; Nausea; Abdominal pain^ |
| Uncommon | Dyspepsia; Constipation; Abdominal distension |
| Hepatobiliary disorders | |
| Common | Elevated liver chemistry tests^# |
| Uncommon | Hepatomegaly; Hepatitis |
| Skin and subcutaneous tissue disorders | |
| Common | Rash^; Pruritus |
| Uncommon | Petechiae; Alopecia; Drug eruption; Dermatitis^ |
| Musculoskeletal and connective tissue disorders | |
| Uncommon | Back pain |
| Renal and urinary disorders | |
| Common | Renal failure |
| General disorders and administration site conditions | |
| Common | Chest pain^; Fatigue |
| Uncommon | Oedema peripheral^; Malaise; Asthenia |
^ Indicates that grouping of appropriate preferred terms into a single medical concept occurred.
* ADR identified post-marketing.
# See section Description of selected adverse reactions below.
Description of selected adverse reactions
Delirium includes reactions of confusional state. Elevated liver chemistry tests includes events of alanine aminotransferase increased, aspartate aminotransferase increased, blood alkaline phosphatase increased, blood bilirubin increased, blood lactate dehydrogenase increased, gamma-glutamyltransferase increased, hepatic enzyme increased, hepatic function abnormal, hyperbilirubinemia, liver function test abnormal, and transaminases increased.
Laboratory effects
In a double-blind, randomized, active-controlled clinical study of 516 patients with invasive fungal disease caused by Aspergillus species or other filamentous fungi, elevated liver transaminases (alanine aminotransferase or aspartate aminotransferase) >3 × Upper Limit of Normal (ULN) were reported at the end of study treatment in 4.4% of patients who received isavuconazole. Marked elevations of liver transaminases >10 × ULN developed in 1.2% of patients on isavuconazole.
Paediatric population
The clinical safety of isavuconazole was assessed in 77 paediatric patients who received at least one dose of intravenous or oral isavuconazole. This included 46 paediatric patients who received isavuconazole as a single dose and who also received other antifungals for prophylaxis, and 31 patients with suspected or confirmed invasive aspergillosis or mucormycosis who received isavuconazole as primary therapy for up to 181 days. Overall, the safety profile of isavuconazole in the paediatric population was similar to that in adults.
Reporting of suspected adverse reactions
Reporting suspected adverse reactions after authorisation of the medicinal product is important. It allows continued monitoring of the benefit/risk balance of the medicinal product. Healthcare professionals are asked to report any suspected adverse reactions via the national reporting system listed in Appendix V.
Incompatibilities
Not applicable.
© All content on this website, including data entry, data processing, decision support tools, "RxReasoner" logo and graphics, is the intellectual property of RxReasoner and is protected by copyright laws. Unauthorized reproduction or distribution of any part of this content without explicit written permission from RxReasoner is strictly prohibited. Any third-party content used on this site is acknowledged and utilized under fair use principles.