IMBRUVICA Hard capsule Ref.[8478] Active ingredients: Ibrutinib
Source: European Medicines Agency (EU) Revision Year: 2025 Publisher: Janssen-Cilag International NV, Turnhoutseweg 30, B-2340, Beerse, Belgium
Pharmacodynamic properties
Pharmacotherapeutic group: Antineoplastic agents, protein kinase inhibitors
ATC code: L01EL01
Mechanism of action
Ibrutinib is a potent, small-molecule inhibitor of Bruton's tyrosine kinase (BTK). Ibrutinib forms a covalent bond with a cysteine residue (Cys-481) in the BTK active site, leading to sustained inhibition of BTK enzymatic activity. BTK, a member of the Tec kinase family, is an important signalling molecule of the B-cell antigen receptor (BCR) and cytokine receptor pathways. The BCR pathway is implicated in the pathogenesis of several B-cell malignancies, including MCL, diffuse large B-cell lymphoma (DLBCL), follicular lymphoma, and CLL. BTK's pivotal role in signalling through the B-cell surface receptors results in activation of pathways necessary for B-cell trafficking, chemotaxis and adhesion. Preclinical studies have shown that ibrutinib effectively inhibits malignant B-cell proliferation and survival in vivo as well as cell migration and substrate adhesion in vitro.
In preclinical tumour models, the combination of ibrutinib and venetoclax resulted in increased cellular apoptosis and anti-tumour activity compared to either agent alone. BTK inhibition by ibrutinib increases CLL cell dependence on BCL-2, a cell survival pathway, while venetoclax inhibits BCL-2 leading to apoptosis.
Lymphocytosis
Upon initiation of treatment, a reversible increase in lymphocyte counts (i.e. ≥50% increase from baseline and an absolute count >5,000/mcL), often associated with reduction of lymphadenopathy, has been observed in about three fourths of patients with CLL treated with IMBRUVICA. This effect has also been observed in about one third of patients with relapsed or refractory MCL treated with IMBRUVICA. This observed lymphocytosis is a pharmacodynamic effect and should not be considered progressive disease in the absence of other clinical findings. In both disease types, lymphocytosis typically occurs during the first month of IMBRUVICA therapy and typically resolves within a median of 8.0 weeks in patients with MCL and 14 weeks in patients with CLL. A large increase in the number of circulating lymphocytes (e.g. >400,000/mcL) has been observed in some patients.
Lymphocytosis was not observed in patients with WM treated with IMBRUVICA.
In vitro platelet aggregation
In an in vitro study, ibrutinib demonstrated inhibition of collagen-induced platelet aggregation. Ibrutinib did not show meaningful inhibition of platelet aggregation using other agonists of platelet aggregation.
Effect on QT/QTc interval and cardiac electrophysiology
The effect of ibrutinib on the QTc interval was evaluated in 20 healthy male and female subjects in a randomised, double-blind thorough QT study with placebo and positive controls. At a supratherapeutic dose of 1 680 mg, ibrutinib did not prolong the QTc interval to any clinically relevant extent. The largest upper bound of the 2-sided 90% CI for the baseline adjusted mean differences between ibrutinib and placebo was below 10 ms. In this same study, a concentration dependent shortening in the QTc interval was observed (-5.3 ms [90% CI: -9.4, -1.1] at a Cmax of 719 ng/mL following the supratherapeutic dose of 1 680 mg).
Clinical efficacy and safety
MCL
Combination treatment in patients previously untreated for MCL who were eligible for autologous stem cell transplantation (ASCT)
The safety and efficacy of IMBRUVICA in patients with previously untreated MCL and who were eligible for autologous stem cell transplantation (ASCT) were evaluated in a randomised, phase 3, multi-centre, open-label, three arm study (TRIANGLE). The TRIANGLE study randomised 870 patients in a 1:1:1 ratio to receive either:
- IMBRUVICA Arm: IMBRUVICA 560 mg daily (Days 1-19) in combination with R-CHOP for three 21-day cycles (Cycles 1, 3, 5) alternating with three 21-day cycles of R-DHAP (Cycles 2, 4, 6) as induction therapy followed by 2 years IMBRUVICA 560 mg daily;
- IMBRUVICA + ASCT Arm: IMBRUVICA 560 mg daily (Days 1-19) in combination with R-CHOP for three 21-day cycles (Cycles 1, 3, 5) alternating with three 21-day cycles of R-DHAP (Cycles 2, 4, 6) as induction therapy followed by high-dose chemotherapy and ASCT followed by 2 years IMBRUVICA 560 mg daily;
- ASCT Arm: R-CHOP for three 21-day cycles (Cycles 1, 3, 5) alternating with three 21-day cycles of R-DHAP (Cycles 2, 4, 6) as induction therapy followed by high-dose chemotherapy and ASCT (Control Arm).
The efficacy analyses were conducted based on 809 patients in the full analysis set (FAS) population using 3 pairwise comparisons of the 3 treatment arms: IMBRUVICA + ASCT vs. ASCT; IMBRUVICA vs. ASCT; and IMBRUVICA + ASCT vs. IMBRUVICA. The FAS population included patients that have either provided explicit permission for their data to be included as per EU General Data Protection Regulation or were deceased. The results presented are from the IMBRUVICA (N=265) arm and the ASCT (N=268) arm, only.
Induction with R-CHOP (rituximab 375 mg/m² on Day 0 or 1, cyclophosphamide 750 mg/m² on Day 1, doxorubicin 50 mg/m² on Day 1, vincristine 1.4 mg/m² up to maximum of 2 mg on Day 1, and prednisone 100 mg on days 1-5) alternating with R-DHAP (rituximab 375 mg/m² on Day 0 or 1, dexamethasone 40 mg on days 1-4, Ara-C 2x 2 g/m² every 12 hours on Day 2, cisplatin 100 mg/m² (alternatively oxaliplatin 130 mg/m²) on Day 1, and G-CSF 5 μg/kg on Day 6) was the same in all 3 treatment arms. Rituximab maintenance therapy was allowed in all treatment groups (59.7% in the IMBRUVICA arm; 62.5% in the ASCT arm) according to national treatment guidelines.
The median age was 57 years (range: 27 to 65 years), 78% were male and 99% were Caucasian. Ninety-eight percent of patients had a baseline ECOG performance status of 0 or 1. At baseline, 86% had Ann Arbor Stage IV disease, and 57%, 28%, and 15% of patients had low, intermediate, and high-risk score by MCL International Prognostic Index (MIPI), respectively. Of the patients 11.6% had blastoid or pleomorphic histology. P53 expression was assessed in 64.6% of patients; expression >50% was present in 14.1% of these patients. Ki-67 proliferation index was assessed in 88.3% of patients and 32.9% of these patients had a proliferation index of >30%.
Tumour response was assessed according to the revised International Working Group (IWG) for non-Hodgkin's lymphoma (NHL) criteria (2007). The primary endpoint was failure-free survival (FFS), defined as the time from randomisation to stable disease at end of induction chemoimmunotherapy, progressive disease, or death from any cause, whichever was earlier.
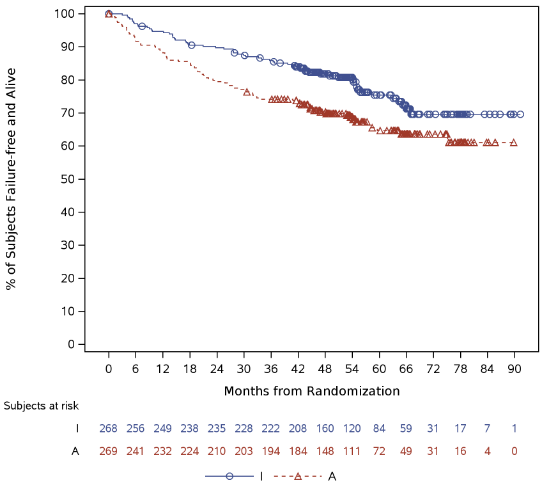
With a median follow-up time on study of 54.9 months, efficacy results for TRIANGLE are shown in Table 4. The Kaplan-Meier curves for FFS and OS are shown in Figures 1 and 2, respectively.
Table 4. Efficacy results in patients with previously untreated MCL (TRIANGLE) (FAS population):
| Endpoint | IMBRUVICA Arm N=268 | ASCT Arm N=269 |
|---|---|---|
| Failure-free survival± | ||
| Number of events (%) | 61 (22.8%) | 87 (32.3%) |
| Stable Disease at the end of induction | 1 (0.4%) | 5 (1.9%) |
| Disease progression | 49 (18.3%) | 60 (22.3%) |
| Death events | 11 (4.1%) | 22 (8.2%) |
| Median (95% CI), months | NE (NE, NE) | NE (NE, NE) |
| IMBRUVICA vs ASCT Arms HR (98.33% CI) (P-value)* | 0.639 (0.428, 0.953) (0.0068) | |
| Overall Survival§ | ||
| Number of deaths (%) | 33 (12.3%) | 60 (22.3%) |
| IMBRUVICA vs ASCT Arms HR (95% CI) (P-value)* | 0.522 (0.341, 0.799) (0.0023) | |
| Overall Response Rate (%)§ (95% CI) | 258 (96.3%) (93.3%, 98.2%) | 248 (92.2%) (88.3%, 95.1%) |
| CR rate (%)§ (95% CI) | 180 (67.2%) (61.2%, 72.8%) | 174 (64.7%) (58.7%, 70.4%) |
FFS=failure-free survival; NE=not estimable; HR=hazard ratio (based on unstratified Cox-regression model); RR=relative risk; CI=confidence interval; CR=complete response; FAS=full analysis set
± The FFS results are not controlled for type 1 error, as these analyses are derived from supplemental analyses conducted for registrational purposes
* Two-sided p-values are from unstratified log-rank test; p-values were tested based on p<0.0167
§ Presented results are derived from descriptive analysis
* I=IMBRUVICA; A=ASCT
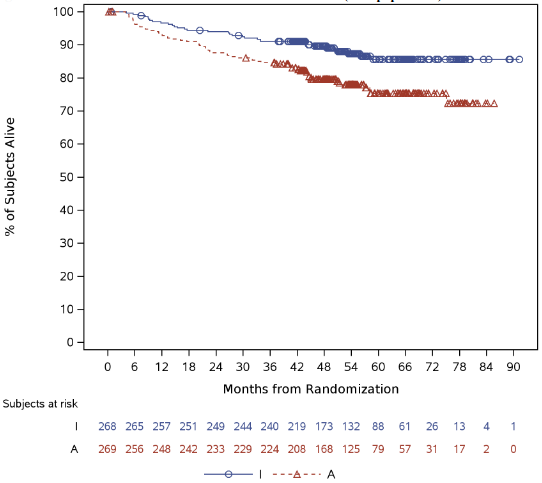
Figure 2. Kaplan-Meier Curve of OS§ in TRIANGLE (FAS population)*:
* I=IMBRUVICA; A=ASCT
§ Presented results are derived from descriptive analysis
Patients with MCL who received at least one prior therapy
Single agent:
The safety and efficacy of IMBRUVICA in patients with relapsed or refractory MCL were evaluated in a single open-label, multi-centre phase 2 study (PCYC-1104-CA) of 111 patients. The median age was 68 years (range: 40 to 84 years), 77% were male and 92% were Caucasian. Patients with ECOG performance status of 3 or greater were excluded from the study. The median time since diagnosis was 42 months, and median number of prior treatments was 3 (range: 1 to 5 treatments), including 35% with prior high-dose chemotherapy, 43% with prior bortezomib, 24% with prior lenalidomide, and 11% with prior autologous or allogeneic stem cell transplant. At baseline, 39% of patients had bulky disease (≥5 cm), 49% had high-risk score by Simplified MCL International Prognostic Index (MIPI), and 72% had advanced disease (extranodal and/or bone marrow involvement) at screening.
IMBRUVICA was administered orally at 560 mg once daily until disease progression or unacceptable toxicity. Tumour response was assessed according to the revised International Working Group (IWG) for non-Hodgkin's lymphoma (NHL) criteria. The primary endpoint in this study was investigator-assessed overall response rate (ORR). Responses to IMBRUVICA are shown in Table 5.
Table 5. ORR and DOR in patients with relapsed or refractory MCL (Study PCYC-1104-CA):
| Total N=111 | |
|---|---|
| ORR (%) | 67.6 |
| 95% CI (%) | (58.0; 76.1) |
| CR (%) | 20.7 |
| PR (%) | 46.8 |
| Median DOR (CR+PR) (months) | 17.5 (15.8, NR) |
| Median time to initial response, months (range) | 1.9 (1.4-13.7) |
| Median time to CR, months (range) | 5.5 (1.7-11.5) |
CI=confidence interval; CR=complete response; DOR=duration of response; ORR=overall response rate; PR=partial response; NR=not reached
The efficacy data was further evaluated by an Independent Review Committee (IRC) demonstrating an ORR of 69%, with a 21% complete response (CR) rate and a 48% partial response (PR) rate. The IRC estimated median DOR was 19.6 months.
The overall response to IMBRUVICA was independent of prior treatment including bortezomib and lenalidomide or underlying risk/prognostic factors, bulky disease, gender or age.
The safety and efficacy of IMBRUVICA were demonstrated in a randomised phase 3, open-label, multicenter study including 280 patients with MCL who received at least one prior therapy (Study MCL3001). Patients were randomised 1:1 to receive either IMBRUVICA orally at 560 mg once daily for 21 days or temsirolimus intravenously at 175 mg on Days 1, 8, 15 of the first cycle followed by 75 mg on Days 1, 8, 15 of each subsequent 21-day cycle. Treatment on both arms continued until disease progression or unacceptable toxicity. The median age was 68 years (range, 34; 88 years), 74% were male and 87% were Caucasian. The median time since diagnosis was 43 months, and median number of prior treatments was 2 (range: 1 to 9 treatments), including 51% with prior high-dose chemotherapy, 18% with prior bortezomib, 5% with prior lenalidomide, and 24% with prior stem cell transplant. At baseline, 53% of patients had bulky disease (≥5 cm), 21% had high-risk score by Simplified MIPI, 60% had extranodal disease and 54% had bone marrow involvement at screening.
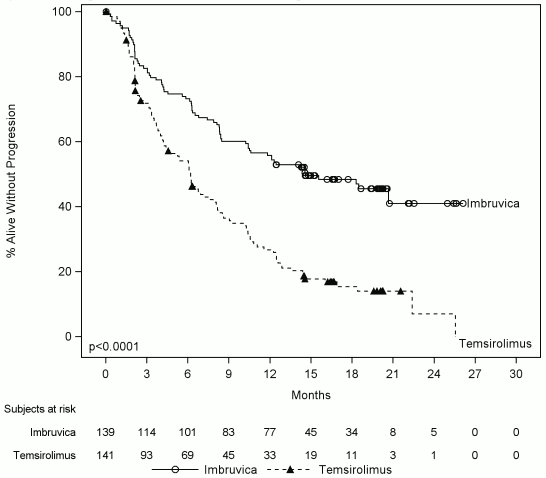
Progression-free survival (PFS) was assessed by IRC according to the revised International Working Group (IWG) for non-Hodgkin's lymphoma (NHL) criteria. Efficacy results for Study MCL3001 are shown in Table 6 and the Kaplan-Meier curve for PFS in Figure 3.
Table 6. Efficacy Results in patients with relapsed or refractory MCL (Study MCL3001):
| Endpoint | IMBRUVICA N=139 | Temsirolimus N=141 |
|---|---|---|
| PFSa | ||
| Median PFS (95% CI), (months) | 14.6 (10.4, NE) | 6.2 (4.2, 7.9) |
| HR=0.43 [95% CI: 0.32, 0.58] | ||
| ORR (%) | 71.9 | 40.4 |
| p-value | p<0.0001 | |
NE = not estimable; HR = hazard ratio; CI = confidence interval; ORR = overall response rate; PFS = progression-free survival
a IRC evaluated.
A smaller proportion of patients treated with ibrutinib experienced a clinically meaningful worsening of lymphoma symptoms versus temsirolimus (27% versus 52%) and time to worsening of symptoms occurred more slowly with ibrutinib versus temsirolimus (HR 0.27, p<0.0001).
Figure 3. Kaplan-Meier Curve of PFS (ITT Population) in Study MCL3001:
CLL
Patients previously untreated for CLL
Single agent:
A randomised, multicenter, open-label phase 3 study (PCYC-1115-CA) of IMBRUVICA versus chlorambucil was conducted in patients with treatment-naïve CLL who were 65 years of age or older. Patients between 65 and 70 years of age were required to have at least one comorbidity that precluded the use of frontline chemo-immunotherapy with fludarabine, cyclophosphamide, and rituximab. Patients (n=269) were randomised 1:1 to receive either IMBRUVICA 420 mg daily until disease progression or unacceptable toxicity, or chlorambucil at a starting dose of 0.5 mg/kg on days 1 and 15 of each 28-day cycle for a maximum of 12 cycles, with an allowance for intrapatient dose increases up to 0.8 mg/kg based on tolerability. After confirmed disease progression, patients on chlorambucil were able to crossover to ibrutinib.
The median age was 73 years (range, 65 to 90 years), 63% were male, and 91% were Caucasian. Ninety one percent of patients had a baseline ECOG performance status of 0 or 1 and 9% had an ECOG performance status of 2. The study enrolled 269 patients with CLL. At baseline, 45% had advanced clinical stage (Rai Stage III or IV), 35% of patients had at least one tumor ≥5 cm, 39% with baseline anemia, 23% with baseline thrombocytopenia, 65% had elevated β2 microglobulin >3500 mcg/L, 47% had a CrCL <60 mL/min, 20% of patients presented with del11q, 6% of patients presented with del17p/tumor protein 53 (TP53) mutation, and 44% of patients presented with unmutated immunoglobulin heavy chain variable region (IGHV).
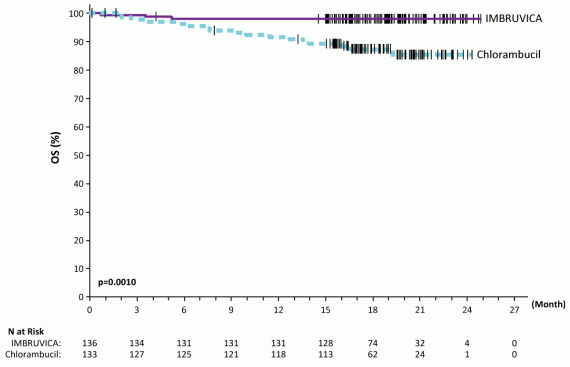
Progression free survival (PFS) as assessed by IRC according to International Workshop on CLL (IWCLL) criteria indicated an 84% statistically significant reduction in the risk of death or progression in the IMBRUVICA arm. Efficacy results for Study PCYC-1115-CA are shown in Table 7 and the Kaplan-Meier curves for PFS and OS are shown in Figures 4 and 5, respectively.
There was a statistically significant sustained platelet or haemoglobin improvement in the ITT population in favour of ibrutinib versus chlorambucil. In patients with baseline cytopenias, sustained haematologic improvement was: platelets 77.1% versus 42.9%; haemoglobin 84.3% versus 45.5% for ibrutinib and chlorambucil, respectively.
Table 7. Efficacy results in Study PCYC-1115-CA:
| Endpoint | IMBRUVICA N=136 | Chlorambucil N=133 |
|---|---|---|
| PFSa | ||
| Number of events (%) | 15 (11.0) | 64 (48.1) |
| Median (95% CI), months | Not reached | 18.9 (14.1, 22.0) |
| HR (95% CI) | 0.161 (0.091, 0.283) | |
| ORRa (CR + PR) | 82.4% | 35.3% |
| P-value | <0.0001 | |
| OSb | ||
| Number of deaths (%) | 3 (2.2) | 17 (12.8) |
| HR (95% CI) | 0.163 (0.048, 0.558) | |
CI = confidence interval; HR = hazard ratio; CR = complete response; ORR = overall response rate; OS = overall survival; PFS = progression-free survival; PR = partial response
a IRC evaluated, median follow-up 18.4 months.
b Median OS not reached for both arms. p<0.005 for OS
Figure 4. Kaplan-Meier curve of PFS (ITT Population) in Study PCYC-1115-CA:
Figure 5. Kaplan-Meier curve of OS (ITT Population) in Study PCYC-1115-CA:
The treatment effect of ibrutinib in Study PCYC-1115-CA was consistent across high-risk patients with del17p/TP53 mutation, del11q, and/or unmutated IGHV.
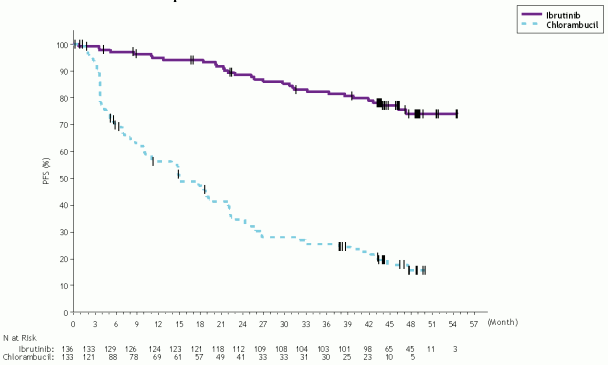
Final analysis at median follow-up of >9 years (115 months):
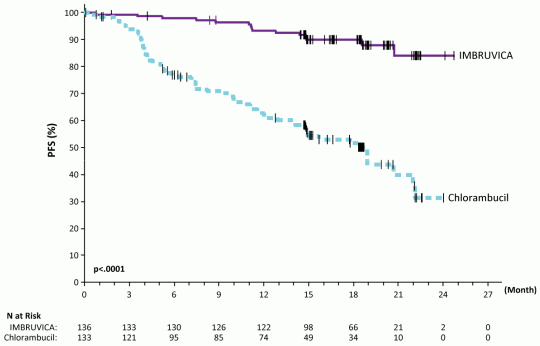
With median follow-up time on study of 115 months in Study PCYC-1115-CA and its extension study, an 85% reduction in the risk of death or progression by investigator assessment was observed for patients in the IMBRUVICA arm. The median investigator-assessed PFS in the IMBRUVICA arm was 107 months and 15 months in the chlorambucil arm; (HR = 0.155 [95% CI (0.110, 0.220)]. The updated Kaplan-Meier curve for PFS is shown in Figure 6. An improvement in ORR was maintained for the ibrutinib arm (91.2%) compared to the chlorambucil arm (36.8%). The complete response rate (CR and CRi) in the IMBRUVICA arm increased from 11% to 36% between the primary analysis and study closure. The Kaplan-Meier landmark estimate for OS at 108 months was 68.0% in the IMBRUVICA arm.
Figure 6. Kaplan-Meier Curve of PFS (ITT Population) in Study PCYC-1115-CA with 115 Months Follow-up:
Combination therapy:
The safety and efficacy of IMBRUVICA in patients with previously untreated CLL/SLL were further evaluated in a randomised, multi-centre, open-label, phase 3 study (PCYC-1130-CA) of IMBRUVICA in combination with obinutuzumab versus chlorambucil in combination with obinutuzumab. The study enrolled patients who were 65 years of age or older or <65 years of age with coexisting medical conditions, reduced renal function as measured by creatinine clearance <70 mL/min, or presence of del17p/TP53 mutation. Patients (n=229) were randomised 1:1 to receive either IMBRUVICA 420 mg daily until disease progression or unacceptable toxicity or chlorambucil at a dose of 0.5 mg/kg on Days 1 and 15 of each 28-day cycle for 6 cycles. In both arms, patients received 1 000 mg of obinutuzumab on Days 1, 8 and 15 of the first cycle, followed by treatment on the first day of 5 subsequent cycles (total of 6 cycles, 28 days each). The first dose of obinutuzumab was divided between day 1 (100 mg) and day 2 (900 mg).
The median age was 71 years (range, 40 to 87 years), 64% were male, and 96% were Caucasian. All patients had a baseline ECOG performance status of 0 (48%) or 1-2 (52%). At baseline, 52% had advanced clinical stage (Rai Stage III or IV), 32% of patients had bulky disease (≥5 cm), 44% with baseline anemia, 22% with baseline thrombocytopenia, 28% had a CrCL <60 mL/min, and the median Cumulative Illness Rating Score for Geriatrics (CIRS-G) was 4 (range, 0 to 12). At baseline, 65% of patients presented with CLL/SLL with high risk factors (del17p/TP53 mutation [18%], del11q [15%], or unmutated IGHV [54%]).
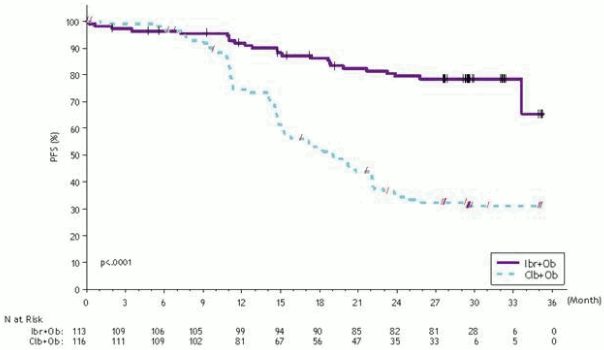
Progression-free survival (PFS) was assessed by IRC according to IWCLL criteria indicated a 77% statistically significant reduction in the risk of death or progression in the IMBRUVICA arm. With a median follow-up time on study of 31 months, the median PFS was not reached in the IMBRUVICA+obinutuzumab arm and was 19 months in the chlorambucil+obinutuzumab arm. Efficacy results for Study PCYC-1130-CA are shown in Table 8 and the Kaplan-Meier curve for PFS is shown in Figure 7.
Table 8. Efficacy results in Study PCYC-1130-CA:
| Endpoint | IMBRUVICA+Obinutuzumab N=113 | Chlorambucil+Obinutuzumab N=116 |
|---|---|---|
| Progression Free Survivala | ||
| Number of events (%) | 24 (21.2) | 74 (63.8) |
| Median (95% CI), months | Not reached | 19.0 (15.1, 22.1) |
| HR (95% CI) | 0.23 (0.15, 0.37) | |
| Overall Response Ratea (%) | 88.5 | 73.3 |
| CRb | 19.5 | 7.8 |
| PRc | 69.0 | 65.5 |
CI=confidence interval; HR=hazard ratio; CR=complete response; PR=partial response.
a IRC evaluated.
b Includes 1 patient in the IMBRUVICA+obinutuzumab arm with a complete response with incomplete marrow recovery (CRi).
c PR=PR+nPR.
Figure 7. Kaplan-Meier Curve of PFS (ITT Population) in Study PCYC-1130-CA:
The treatment effect of ibrutinib was consistent across the high-risk CLL/SLL population (del17p/TP53 mutation, del11q, or unmutated IGHV), with a PFS HR of 0.15 [95% CI (0.09, 0.27)], as shown in Table 9. The 2-year PFS rate estimates for the high-risk CLL/SLL population were 78.8% [95% CI (67.3, 86.7)] and 15.5% [95% CI (8.1, 25.2)] in the IMBRUVICA+obinutuzumab and chlorambucil+obinutuzumab arms, respectively.
Table 9. Subgroup analysis of PFS (Study PCYC-1130-CA):
| N | Hazard Ratio | 95% CI | |
|---|---|---|---|
| All subjects | 229 | 0,231 | 0,145, 0,367 |
| High risk (del17p/TP53/del11q/unmutated IGHV) | |||
| Yes | 148 | 0,154 | 0,087, 0,270 |
| Noo | 81 | 0,521 | 0,221, 1,231 |
| Del17p/TP53 | |||
| Yes | 41 | 0,109 | 0,031, 0,380 |
| No | 188 | 0,275 | 0,166, 0,455 |
| FISH | |||
| Del17p | 32 | 0,141 | 0,039, 0,506 |
| Del11q | 35 | 0,131 | 0,030, 0,573 |
| Others | 162 | 0,302 | 0,176, 0,520 |
| Unmutated IGHV | |||
| Yes | 123 | 0,150 | 0,084, 0,269 |
| No | 91 | 0,300 | 0,120, 0,749 |
| Age | |||
| <65 | 46 | 0,293 | 0,122, 0,705 |
| ≥65 | 183 | 0,215 | 0,125, 0,372 |
| Bulky disease | |||
| <5 cm | 154 | 0,289 | 0,161, 0,521 |
| ≥5 cm | 74 | 0,184 | 0,085, 0,398 |
| Rai stage | |||
| 0/I/II | 110 | 0,221 | 0,115, 0,424 |
| III/IV | 119 | 0,246 | 0,127, 0,477 |
| ECOG per CRF | |||
| 0 | 110 | 0,226 | 0,110, 0,464 |
| 1-2 | 119 | 0,239 | 0,130, 0,438 |
Hazard ratio based on non-stratified analysis
Any grade infusion-related reactions were observed in 25% of patients treated with IMBRUVICA+obinutuzumab and 58% of patients treated with chlorambucil+obinutuzumab. Grade 3 or higher or serious infusion-related reactions were observed in 3% of patients treated with IMBRUVICA+obinutuzumab and 9% of patients treated with chlorambucil+obinutuzumab.
The safety and efficacy of IMBRUVICA in patients with previously untreated CLL or SLL were further evaluated in a randomised, multi-centre, open-label, phase 3 study (E1912) of IMBRUVICA in combination with rituximab (IR) versus standard fludarabine, cyclophosphamide, and rituximab (FCR) chemo-immunotherapy. The study enrolled previously untreated patients with CLL or SLL who were 70 years or younger. Patients with del17p were excluded from the study. Patients (n=529) were randomised 2:1 to receive either IR or FCR. IMBRUVICA was administered at a dose of 420 mg daily until disease progression or unacceptable toxicity. Fludarabine was administered at a dose of 25 mg/m², and cyclophosphamide was administered at a dose of 250 mg/m², both on Days 1, 2, and 3 of Cycles 1-6. Rituximab was initiated in Cycle 2 for the IR arm and in Cycle 1 for the FCR arm and was administered at a dose of 50 mg/m² on Day 1 of the first cycle, 325 mg/m² on Day 2 of the first cycle, and 500 mg/m² on Day 1 of 5 subsequent cycles, for a total of 6 cycles. Each cycle was 28 days.
The median age was 58 years (range, 28 to 70 years), 67% were male, and 90% were Caucasian. All patients had a baseline ECOG performance status of 0 or 1 (98%) or 2 (2%). At baseline, 43% of patients presented with Rai Stage III or IV, and 59% of patients presented with CLL/SLL with high risk factors (TP53 mutation [6%], del11q [22%], or unmutated IGHV [53%]).
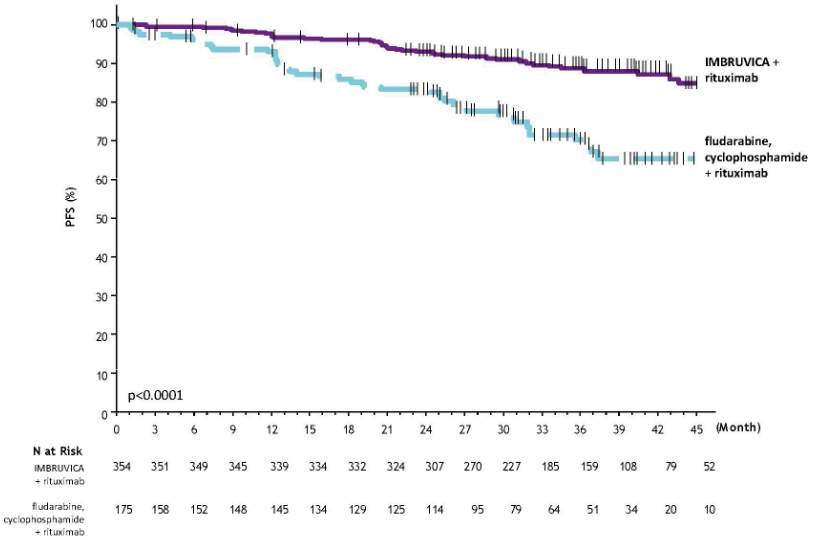
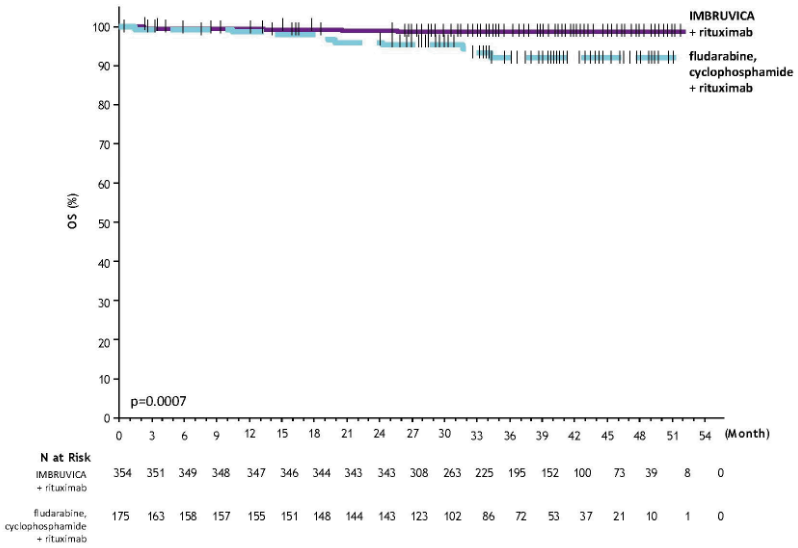
With a median follow-up time on study of 37 months, efficacy results for E1912 are shown in Table 10. The Kaplan-Meier curves for PFS, assessed according to IWCLL criteria, and OS are shown in Figures 8 and 9, respectively.
Table 10. Efficacy results in Study E1912:
| Endpoint | Ibrutinib+rituximab (IR) N=354 | Fludarabine, Cyclophosphamide, and Rituximab (FCR) N=175 |
|---|---|---|
| Progression-Free Survival | ||
| Number of events (%) | 41 (12) | 44 (25) |
| Disease progression | 39 | 38 |
| Death events | 2 | 6 |
| Median (95% CI), months | NE (49.4, NE) | NE (47.1, NE) |
| HR (95% CI) | 0.34 (0.22, 0.52) | |
| P-valuea | <0.0001 | |
| Overall Survival | ||
| Number of deaths (%) | 4 (1) | 10 (6) |
| HR (95% CI) | 0.17 (0.05, 0.54) | |
| P-valuea | 0.0007 | |
| Overall Response Rateb (%) | 96.9 | 85.7 |
a P-value is from unstratified log-rank test.
Figure 8. Kaplan-Meier Curve of PFS (ITT Population) in Study E1912:
The treatment effect of ibrutinib was consistent across the high-risk CLL/SLL population (TP53 mutation, del11q, or unmutated IGHV), with a PFS HR of 0.23 [95% CI (0.13, 0.40)], p<0.0001, as shown in Table 11. The 3-year PFS rate estimates for the high-risk CLL/SLL population were 90.4% [95% CI (85.4, 93.7)] and 60.3% [95% CI (46.2, 71.8)] in the IR and FCR arms, respectively.
Table 11. Subgroup analysis of PFS (Study E1912):
| N | Hazard Ratio | 95% CI | |
|---|---|---|---|
| All subjects | 529 | 0.340 | 0.222, 0.522 |
| High risk (TP53/del11q/unmutated IGHV) | |||
| Yes | 313 | 0.231 | 0.132, 0.404 |
| No | 216 | 0.568 | 0.292, 1.105 |
| del11q | |||
| Yes | 117 | 0.199 | 0.088, 0.453 |
| No | 410 | 0.433 | 0.260, 0.722 |
| Unmutated IGHV | |||
| Yes | 281 | 0.233 | 0.129, 0.421 |
| No | 112 | 0.741 | 0.276, 1.993 |
| Bulky disease | |||
| <5 cm | 316 | 0.393 | 0.217, 0.711 |
| ≥5 cm | 194 | 0.257 | 0.134, 0.494 |
| Rai stage | |||
| 0/I/II | 301 | 0.398 | 0.224, 0.708 |
| III/IV | 228 | 0.281 | 0.148, 0.534 |
| ECOG | |||
| 0 | 335 | 0.242 | 0.138, 0.422 |
| 1-2 | 194 | 0.551 | 0.271, 1.118 |
Hazard ratio based on non-stratified analysis
Figure 9. Kaplan-Meier Curve of OS (ITT Population) in Study E1912:
Fixed duration combination therapy:
The safety and efficacy of fixed duration therapy with IMBRUVICA in combination with venetoclax versus chlorambucil in combination with obinutuzumab in patients with previously untreated CLL were evaluated in a randomised, open-label, phase 3 (CLL3011) study. The study enrolled patients with previously untreated CLL who were 65 years or older, and adult patients <65 years of age with a CIRS score >6 or CrCL ≥30 to <70 mL/min. Patients with del 17p or known TP53 mutations were excluded. Patients (n=211) were randomised 1:1 to receive either IMBRUVICA in combination with venetoclax or chlorambucil in combination with obinutuzumab. Patients in the IMBRUVICA plus venetoclax arm received single agent IMBRUVICA for 3 cycles followed by IMBRUVICA in combination with venetoclax for 12 cycles (including 5-week dose-titration schedule). Each cycle was 28 days. IMBRUVICA was administered at a dose of 420 mg daily. Venetoclax was administered daily, starting with 20 mg for 1 week, followed by 1 week at each dose level of 50 mg, 100 mg, and 200 mg, then the recommended daily dose of 400 mg. Patients randomised to the chlorambucil plus obinutuzumab arm received treatment for 6 cycles. Obinutuzumab was administered at a dose of 1 000 mg on Days 1, 8 and 15 in Cycle 1. In Cycles 2 to 6, 1 000 mg obinutuzumab was given on Day 1. Chlorambucil was administered at a dose of 0.5 mg/kg body weight on Days 1 and 15 of Cycles 1 to 6. Patients with confirmed progression by IWCLL criteria after completion of either fixed duration regimen could be treated with single-agent IMBRUVICA.
The median age was 71 years (range, 47 to 93 years), 58% were male, and 96% were Caucasian. All patients had a baseline ECOG performance status of 0 (35%), 1 (53%), or 2 (12%). At baseline, 18% of patients presented with CLL with del 11q and 52% with unmutated IGHV.
At baseline assessment for risk of tumour lysis syndrome, 25% of patients had high tumour burden. After 3 cycles of single-agent IMBRUVICA lead-in therapy, 2% of patients had high tumour burden. High tumour burden was defined as any lymph node ≥10 cm; or any lymph node ≥5 cm and absolute lymphocyte count ≥25×109/L.
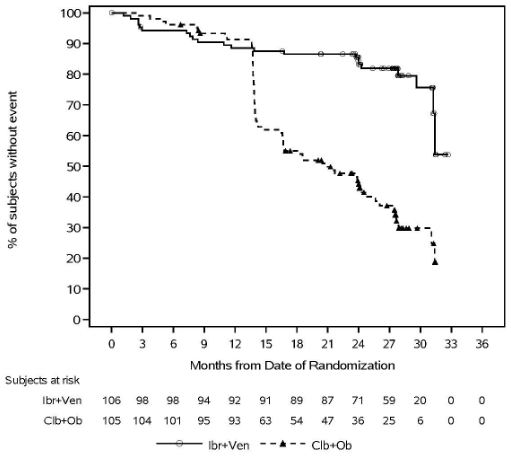
With a median follow-up time on study of 28 months, efficacy results for Study CLL3011 assessed by an IRC according to IWCLL criteria are shown in Table 12, the Kaplan-Meier curve for PFS is shown in Figure 10, and rates of minimal residual disease (MRD) negativity are shown in Table 13.
Table 12. Efficacy results in Study CLL3011:
| Endpointa | IMBRUVICA + Venetoclax N=106 | Chlorambucil + Obinutuzumab N=105 |
|---|---|---|
| Progression-Free Survival | ||
| Number of events (%) | 22 (20.8) | 67 (63.8) |
| Median (95% CI), months | NE (31.2, NE) | 21.0 (16.6, 24.7) |
| HR (95% CI) | 0.22 (0.13, 0.36) | |
| P-valueb | <0.0001 | |
| Complete Response Rate (%)c | 38.7 | 11.4 |
| 95% CI | (29.4, 48.0) | (5.3, 17.5) |
| P-valued | <0.0001 | |
| Overall Response Rate (%)e | 86.8 | 84.8 |
| 95% CI | (80.3, 93.2) | (77.9, 91.6) |
a Based on IRC assessment
b P-value is from stratified log-rank test
c Includes 3 patients in the IMBRUVICA + venetoclax arm with a complete response with incomplete marrow recovery (CRi)
d P-value is from Cochran-Mantel-Haenszel chi-square test
e Overall response = CR+CRi+nPR+PR
CR = complete response; CRi = complete response with incomplete marrow recovery; HR = hazard ratio; NE = not evaluable; nPR = nodular partial response; PR = partial response
Figure 10. Kaplan-Meier Curve of Progression-Free Survival (ITT Population) in Patients with CLL in Study CLL3011:
The treatment effect of IMBRUVICA plus venetoclax was consistent across the high-risk CLL population (TP53 mutation, del 11q, or unmutated IGHV), with a PFS HR of 0.23 [95% CI (0.13, 0.41)].
Overall survival data were not mature. With a median follow-up of 28 months, there was no significant difference between treatment arms with a total of 23 deaths: 11 (10.4%) in the IMBRUVICA plus venetoclax arm and 12 (11.4%) in the chlorambucil plus obinutuzumab arm with a OS HR of 1.048 [95% CI (0.454, 2.419)]. After 6 months additional follow-up, 11 (10.4%) and 16 (15.2%) deaths were reported in the IMBRUVICA plus venetoclax arm and the chlorambucil plus obinutuzumab arm, respectively with OS HR estimated at 0.760 [95% CI (0.352, 1.642]).
Table 13. Minimal residual disease negativity rates in Study CLL3011:
| NGS Assaya | Flow cytometryb | |||
|---|---|---|---|---|
| IMBRUVICA + Venetoclax N=106 | Chlorambucil + Obinutuzumab N=105 | IMBRUVICA + Venetoclax N=106 | Chlorambucil + Obinutuzumab N=105 | |
| MRD Negativity Rate | ||||
| Bone marrow, n (%) | 59 (55.7) | 22 (21.0) | 72 (67.9) | 24 (22.9) |
| 95% CI | (46.2, 65.1) | (13.2, 28.7) | (59.0, 76.8) | (14.8, 30.9) |
| P-value | <0.0001 | |||
| Peripheral Blood, n (%) | 63 (59.4) | 42 (40.0) | 85 (80.2) | 49 (46.7) |
| 95% CI | (50.1, 68.8) | (30.6, 49.4) | (72.6, 87.8) | (37.1, 56.2) |
| MRD Negativity Rate at Three Months After Completion of Treatment | ||||
| Bone marrow, n (%) | 55 (51.9) | 18 (17.1) | 60 (56.6) | 17 (16.2) |
| 95% CI | (42.4, 61.4) | (9.9, 24.4) | (47.2, 66.0) | 9.1, 23.2) |
| Peripheral Blood, n (%) | 58 (54.7) | 41 (39.0) | 65 (61.3) | 43 (41.0) |
| 95% CI | (45.2, 64.2) | (29.7, 48.4) | (52.0, 70.6) | 31.5, 50.4) |
P-values are from Cochran-Mantel-Haenszel chi-square test. P-value for MRD negativity rate in bone marrow by NGS was the primary MRD analysis.
a Based on threshold of 10-4 using a next-generation sequencing assay (clonoSEQ)
b MRD was evaluated by flow cytometry of peripheral blood or bone marrow per central laboratory. The definition of negative status was <1 CLL cell per 10 000 leukocytes (<1×104).
CI = confidence interval; NGS = next-generation sequencing
Twelve months after the completion of treatment, MRD negativity rates in peripheral blood were 49.1% (52/106) by NGS assay and 54.7% (58/106) by flow cytometry in patients treated with IMBRUVICA plus venetoclax and, at the corresponding time point, was 12.4% (13/105) by NGS assay and 16.2% (17/105) by flow cytometry in patients treated with chlorambucil plus obinutuzumab.
TLS was reported in 6 patients treated with chlorambucil plus obinutuzumab and no TLS was reported in IMBRUVICA in combination with venetoclax.
Median follow-up of 64 months:
With a median follow-up time on study of 64.0 months in Study CLL3011, a 73% reduction in the risk of death or progression by investigator assessment was observed for patients in the IMBRUVICA arm. The PFS hazard ratio was 0.267 [95% CI (0.182, 0.393), nominal p<0.0001, not type 1 error controlled]. There were 20 (18.9%) deaths in the IMBRUVICA plus venetoclax arm and 40 (38.1%) in the chlorambucil plus obinutuzumab arm corresponding to a HR of 0.462 (95% CI: 0.269, 0.791, nominal p=0.0039, not type 1 error controlled). Median time to next treatment was not reached for IMBRUVICA plus venetoclax arm and was 65 months for chlorambucil plus obinutuzumab arm (HR=0.233; 95% CI: 0.130, 0.416) with 15.1% of subjects in the IMBRUVICA plus venetoclax arm and 43.8% of subjects in the chlorambucil plus obinutuzumab arm having initiated subsequent anticancer therapy.
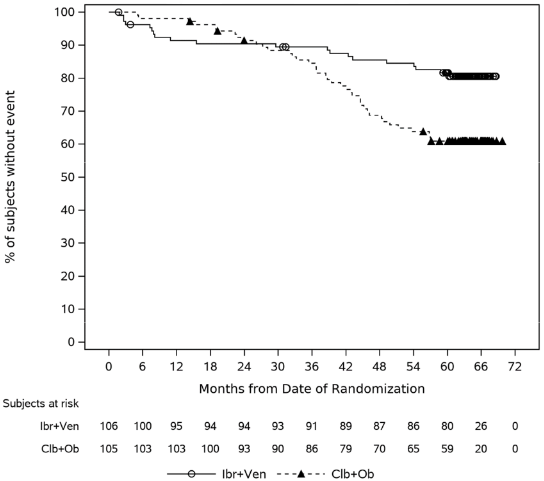
Kaplan-Meier curve for OS is shown in Figure 11.
Figure 11. Kaplan-Meier Curve of Overall Survival (ITT Population) in Patients with CLL/SLL in Study CLL3011 at 64 Months Follow-up:
The safety and efficacy of fixed duration therapy with IMBRUVICA in combination with venetoclax in patients with previously untreated CLL were further evaluated in a cohort of the phase 2, multi-centre, 2-cohort study (PCYC-1142-CA). The study enrolled previously untreated patients with CLL who were 70 years or younger. The study enrolled 323 patients, of these, 159 patients were enrolled to fixed duration therapy consisting of 3 cycles of single agent IMBRUVICA followed by IMBRUVICA in combination with venetoclax for 12 cycles (including 5-week dose titration schedule). Each cycle was 28 days. IMBRUVICA was administered at a dose of 420 mg daily. Venetoclax was administered daily, starting with 20 mg for 1 week, followed by 1 week at each dose level of 50 mg, 100 mg, and 200 mg, then the recommended daily dose of 400 mg. Patients with confirmed progression by IWCLL criteria after completion of the fixed duration regimen could be retreated with single-agent IMBRUVICA.
The median age was 60 years (range, 33 to 71 years), 67% were male, and 92% were Caucasian. All patients had a baseline ECOG performance status of 0 (69%) or 1 (31%). At baseline, 13% of patients had del 17p, 18% with del 11q, 17% with del 17p/TP53 mutation, 56% with unmutated IGHV and 19% with complex karyotype. At baseline assessment for risk of tumour lysis syndrome, 21% of patients had high tumour burden.
After 3 cycles of single-agent IMBRUVICA lead-in therapy, 1% of patients had high tumour burden. High tumour burden was defined as any lymph node ≥10 cm, or any lymph node ≥5 cm and absolute lymphocyte count ≥25×109/L.
With a median follow-up time on study of 28 months, efficacy results for PCYC-1142-CA assessed by an IRC according to IWCLL criteria are shown in Table 14, and rates of minimal residual disease (MRD) negativity are shown in Table 15.
| Endpointa | IMBRUVICA + Venetoclax | |
|---|---|---|
| Without Del 17p (N=136) | All (N=159) | |
| Overall Response Rate, n (%)b | 130 (95.6) | 153 (96.2) |
| 95% CI (%) | (92.1, 99.0) | (93.3, 99.2) |
| Complete Response Rate, n (%)c | 83 (61.0) | 95 (59.7) |
| 95% CI (%) | (52.8, 69.2) | (52.1, 67.4) |
| Median duration of CR, months (range)d | NE (0.03+, 24.9+) | NE (0.03+, 24.9+) |
a Based on IRC assessment
b Overall response = CR + CRi + nPR + PR
c Includes 3 patients with a complete response with incomplete marrow recovery (CRi)
^d6 A '+' sign indicates a censored observation
CR = complete response; CRi = complete response with incomplete marrow recovery; nPR = nodular partial response;
PR = partial response; NE = not evaluable
Table 15. Minimal residual disease negativity rates in Study PCYC 1142-CA (Fixed duration cohort):
| Endpoint | IMBRUVICA + Venetoclax | |
|---|---|---|
| Without Del 17p (N=136) | All (N=159) | |
| MRD Negativity Rate | ||
| Bone marrow, n (%) | 84 (61.8) | 95 (59.7) |
| 95% CI | (53.6, 69.9) | (52.1, 67.4) |
| Peripheral Blood, n (%) | 104 (76.5) | 122 (76.7) |
| 95% CI | (69.3, 83.6) | (70.2, 83.3) |
| MRD Negativity Rate at Three Months After Completion of Treatment | ||
| Bone marrow, n (%) | 74 (54.4) | 83 (52.2) |
| 95% CI | (46.0, 62.8) | (44.4, 60.0) |
| Peripheral Blood, n (%) | 78 (57.4) | 90 (56.6) |
| 95% CI | (49.0, 65.7) | (48.9, 64.3) |
MRD was evaluated by flow cytometry of peripheral blood or bone marrow per central laboratory. The definition of negative status was <1 CLL cell per 10 000 leukocytes (<1×104).
CI = confidence interval
In patients with del 17p/TP53 mutation (n=27) in PCYC-1142-CA the overall response rate based on IRC assessment was 96.3%; complete response rate was 55.6% and the median duration of complete response was not reached (range, 4.3 to 22.6 months). The MRD negativity rate in patients with del 17p/TP53 mutation 3 months after completion of treatment in bone marrow and peripheral blood was 40.7% and 59.3%, respectively.
No TLS was reported in patients treated with IMBRUVICA in combination with venetoclax.
Patients with CLL who received at least one prior therapy
Single agent:
The safety and efficacy of IMBRUVICA in patients with CLL were demonstrated in one uncontrolled study and one randomised, controlled study. The open-label, multi-centre study (PCYC-1102-CA) included 51 patients with relapsed or refractory CLL, who received 420 mg once daily. IMBRUVICA was administered until disease progression or unacceptable toxicity. The median age was 68 years (range: 37 to 82 years), median time since diagnosis was 80 months, and median number of prior treatments was 4 (range: 1 to 12 treatments), including 92.2% with a prior nucleoside analogue, 98.0% with prior rituximab, 86.3% with a prior alkylator, 39.2% with prior bendamustine and 19.6% with prior ofatumumab. At baseline, 39.2% of patients had Rai Stage IV, 45.1% had bulky disease (≥5 cm), 35.3% had deletion 17p and 31.4% had deletion 11q.
ORR was assessed according to the 2008 IWCLL criteria by investigators and IRC. At a median duration follow-up of 16.4 months, the ORR by IRC for the 51 relapsed or refractory patients was 64.7% (95% CI: 50.1%; 77.6%), all PRs. The ORR including PR with lymphocytosis was 70.6%. Median time to response was 1.9 months. The DOR ranged from 3.9 to 24.2+ months. The median DOR was not reached.
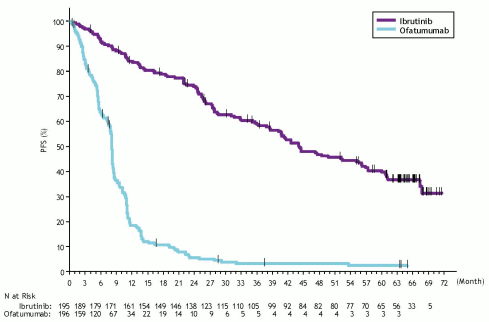
A randomised, multi-centre, open-label phase 3 study of IMBRUVICA versus ofatumumab (PCYC-1112-CA) was conducted in patients with relapsed or refractory CLL. Patients (n=391) were randomised 1:1 to receive either IMBRUVICA 420 mg daily until disease progression or unacceptable toxicity, or ofatumumab for up to 12 doses (300/2 000 mg). Fifty-seven patients randomised to ofatumumab crossed over following progression to receive IMBRUVICA. The median age was 67 years (range: 30 to 88 years), 68% were male, and 90% were Caucasian. All patients had a baseline ECOG performance status of 0 or 1. The median time since diagnosis was 91 months and the median number of prior treatments was 2 (range: 1 to 13 treatments). At baseline, 58% of patients had at least one tumour ≥5 cm. Thirty-two percent of patients had deletion 17p (with 50% of patients having deletion 17p/TP53 mutation), 24% had 11q deletion, and 47% of patients had unmutated IGHV.
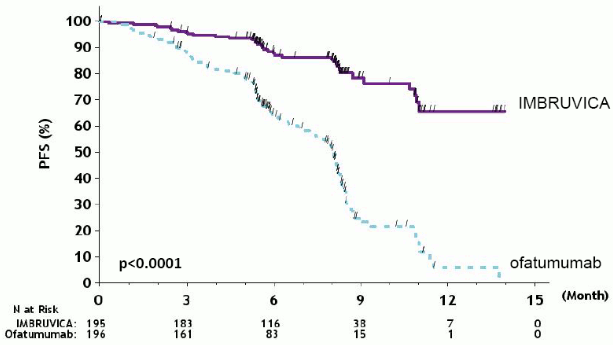
Progression-free survival (PFS) as assessed by an IRC according to IWCLL criteria indicated a 78% statistically significant reduction in the risk of death or progression for patients in the IMBRUVICA arm. Analysis of OS demonstrated a 57% statistically significant reduction in the risk of death for patients in the IMBRUVICA arm. Efficacy results for Study PCYC-1112-CA are shown in Table 16.
Table 16. Efficacy results in patients with CLL (Study PCYC-1112-CA):
| Endpoint | IMBRUVICA N=195 | Ofatumumab N=196 |
|---|---|---|
| Median PFS | Not reached | 8.1 months |
| HR=0.215 [95% CI: 0.146; 0.317] | ||
| OSa | HR=0.434 [95% CI: 0.238; 0.789]b HR=0.387 [95% CI: 0.216; 0.695]c | |
| ORRd,e (%) | 42.6 | 4.1 |
| ORR including PR with lymphocytosisd (%) | 62.6 | 4.1 |
HR = hazard ratio; CI = confidence interval; ORR = overall response rate; OS = overall survival; PFS = progression-free survival; PR = partial response
a Median OS not reached for both arms. p<0.005 for OS.
b Patients randomised to ofatumumab were censored when starting IMBRUVICA if applicable.
c Sensitivity analysis in which crossover patients from the ofatumumab arm were not censored at the date of first dose of IMBRUVICA.
d Per IRC. Repeat CT scans required to confirm response.
e All PRs achieved; p<0.0001 for ORR.
Median follow-up time on study=9 months
The efficacy was similar across all of the subgroups examined, including in patients with and without deletion 17p, a pre-specified stratification factor (Table 17).
Table 17. Subgroup analysis of PFS (Study PCYC-1112-CA):
| N | Hazard Ratio | 95% CI | |
|---|---|---|---|
| All subjects | 391 | 0,210 | (0,143, 0,308) |
| Del17P | |||
| Yes | 127 | 0,247 | (0,136, 0,450) |
| No | 264 | 0,194 | (0,117, 0,323) |
| Refractory disease to purine analog | |||
| Yes | 175 | 0,178 | (0,100, 0,320) |
| No | 216 | 0,242 | (0,145, 0,404) |
| Age | |||
| <65 | 152 | 0,166 | (0,088, 0,315) |
| ≥65 | 239 | 0,243 | (0,149, 0,395) |
| Number of prior lines | |||
| <3 | 198 | 0,189 | (0,100, 0,358) |
| ≥3 | 193 | 0,212 | (0,130, 0,344) |
| Bulky disease | |||
| <5 cm | 163 | 0,237 | (0,127, 0,442) |
| ≥5 cm | 225 | 0,191 | (0,117, 0,311) |
Hazard ratio based on non-stratified analysis.
The Kaplan-Meier curve for PFS is shown in Figure 12.
Figure 12. Kaplan-Meier curve of PFS (ITT Population) in Study PCYC-1112-CA:
Final Analysis at 65-month follow-up:
With a median follow-up time on study of 65 months in Study PCYC-1112-CA, an 85% reduction in the risk of death or progression by investigator assessment was observed for patients in the IMBRUVICA arm. The median investigator-assessed PFS according to IWCLL criteria was 44.1 months [95% CI (38.47, 56.18)] in the IMBRUVICA arm and 8.1 months [95% CI (7.79, 8.25)] in the ofatumumab arm, respectively; HR=0.15 [95% CI (0.11, 0.20)]. The updated Kaplan-Meier curve for PFS is shown in Figure 13. The investigator-assessed ORR in the IMBRUVICA arm was 87.7% versus 22.4% in the ofatumumab arm. At the time of final analysis, 133 (67.9%) of the 196 subjects originally randomised to the ofatumumab treatment arm had crossed over to ibrutinib treatment. The median investigator-assessed PFS2 (time from randomisation until PFS event after first subsequent anti-neoplastic therapy) according to IWCLL criteria was 65.4 months [95% CI (51.61, not estimable)] in the IMBRUVICA arm and 38.5 months [95% CI (19.98, 47.24)] in the ofatumumab arm, respectively; HR=0.54 [95% CI (0.41, 0.71)]. The median OS was 67.7 months [95% CI (61.0, not estimable)] in the IMBRUVICA arm.
The treatment effect of ibrutinib in Study PCYC-1112-CA was consistent across high-risk patients with deletion 17p/TP53 mutation, deletion 11q, and/or unmutated IGHV.
Figure 13. Kaplan-Meier Curve of PFS (ITT Population) in Study PCYC-1112-CA at Final Analysis with 65 Months Follow-up:
Combination therapy:
The safety and efficacy of IMBRUVICA in patients previously treated for CLL were further evaluated in a randomised, multi-centre, double-blinded phase 3 study of IMBRUVICA in combination with BR versus placebo+BR (Study CLL3001). Patients (n=578) were randomised 1:1 to receive either IMBRUVICA 420 mg daily or placebo in combination with BR until disease progression, or unacceptable toxicity. All patients received BR for a maximum of six 28-day cycles. Bendamustine was dosed at 70 mg/m² infused IV over 30 minutes on Cycle 1, Days 2 and 3, and on Cycles 2-6, Days 1 and 2 for up to 6 cycles. Rituximab was administered at a dose of 375 mg/m² in the first cycle, Day 1, and 500 mg/m² Cycles 2 through 6, Day 1. Ninety patients randomised to placebo+BR crossed over to receive IMBRUVICA following IRC confirmed progression. The median age was 64 years (range, 31 to 86 years), 66% were male, and 91% were Caucasian. All patients had a baseline ECOG performance status of 0 or 1. The median time since diagnosis was 6 years and the median number of prior treatments was 2 (range, 1 to 11 treatments). At baseline, 56% of patients had at least one tumour ≥5 cm, 26% had del11q.
Progression-free survival (PFS) was assessed by IRC according to IWCLL criteria. Efficacy results for Study CLL3001 are shown in Table 18.
Table 18. Efficacy Results in patients with CLL (Study CLL3001):
| Endpoint | IMBRUVICA+BR N=289 | Placebo+BR N=289 |
|---|---|---|
| PFSa | ||
| Median (95% CI), months | Not reached | 13.3 (11.3, 13.9) |
| HR=0.203 [95% CI: 0.150, 0.276] | ||
| ORRb % | 82.7 | 67.8 |
| OSc | HR=0.628 [95% CI: 0.385, 1.024] | |
CI=confidence interval; HR=hazard ratio; ORR=overall response rate; OS=overall survival; PFS=progression-free survival
a IRC evaluated.
b IRC evaluated, ORR (complete response, complete response with incomplete marrow recovery, nodular partial response, partial response).
c Median OS not reached for both arms.
WM
Single agent:
The safety and efficacy of IMBRUVICA in WM (IgM-excreting lymphoplasmacytic lymphoma) were evaluated in an open-label, multi-centre, single-arm trial of 63 previously treated patients. The median age was 63 years (range: 44 to 86 years), 76% were male, and 95% were Caucasian. All patients had a baseline ECOG performance status of 0 or 1. The median time since diagnosis was 74 months, and the median number of prior treatments was 2 (range: 1 to 11 treatments). At baseline, the median serum IgM value was 3.5 g/dL, and 60% of patients were anaemic (haemoglobin ≤11 g/dL or 6.8 mmol/L).
IMBRUVICA was administered orally at 420 mg once daily until disease progression or unacceptable toxicity. The primary endpoint in this study was ORR per investigator assessment. The ORR and DOR were assessed using criteria adopted from the Third International Workshop of WM. Responses to IMBRUVICA are shown in Table 19.
Table 19. ORR and DOR in patients with WM:
| Total (N=63) | |
|---|---|
| ORR (%) | 87.3 |
| 95% CI (%) | (76.5, 94.4) |
| VGPR (%) | 14.3 |
| PR (%) | 55.6 |
| MR (%) | 17.5 |
| Median DOR months (range) | NR (0.03+, 18.8+) |
CI = confidence interval; DOR = duration of response; NR = not reached; MR = minor response; PR = partial response; VGPR = very good partial response; ORR = MR + PR + VGPR
Median follow-up time on study = 14.8 months
The median time to response was 1.0 month (range: 0.7-13.4 months). Efficacy results were also assessed by an IRC demonstrating an ORR of 83%, with a 11% VGPR rate and a 51% PR rate.
Combination therapy:
The safety and efficacy of IMBRUVICA in WM were further evaluated in patients with treatment-naïve or previously treated WM in a randomised, multi-centre, double-blinded phase 3 study of IMBRUVICA in combination with rituximab versus placebo in combination with rituximab (PCYC-1127-CA). Patients (n=150) were randomised 1:1 to receive either IMBRUVICA 420 mg daily or placebo in combination with rituximab until disease progression or unacceptable toxicity. Rituximab was administered weekly at a dose of 375 mg/m² for 4 consecutive weeks (weeks 1-4) followed by a second course of weekly rituximab for 4 consecutive weeks (weeks 17-20).
The median age was 69 years (range, 36 to 89 years), 66% were male, and 79% were Caucasian. Ninety-three percent of patients had a baseline ECOG performance status of 0 or 1, and 7% of patients had a baseline ECOG performance status of 2. Forty-five percent of patients were treatment-naïve, and 55% of patients were previously treated. The median time since diagnosis was 52.6 months (treatment-naïve patients=6.5 months and previously treated patients=94.3 months). Among previously treated patients, the median number of prior treatments was 2 (range, 1 to 6 treatments). At baseline, the median serum IgM value was 3.2 g/dL (range, 0.6 to 8.3 g/dL), 63% of patients were anaemic (haemoglobin ≤11 g/dL or 6.8 mmol/L) and MYD88 L265P mutations were present in 77% of patients, absent in 13% of patients, and 9% of patients were not evaluable for mutation status.
At the primary analysis, with a median follow-up of 26.5 months, the IRC-assessed PFS hazard ratiowas 0.20 [95% CI (0.11, 0.38)]. PFS hazard ratios for treatment-naïve patients, previously treated patients, and patients with or without MYD88 L265P mutations were consistent with the PFS hazard ratio for the ITT population.
Grade 3 or 4 infusion-related reactions were observed in 1% of patients treated with IMBRUVICA+rituximab and 16% of patients treated with placebo+rituximab.
Tumour flare in the form of IgM increase occurred in 8.0% of subjects in the IMBRUVICA+rituximab arm and 46.7% of subjects in the placebo+rituximab arm.
Final Analysis at 63-month follow-up:
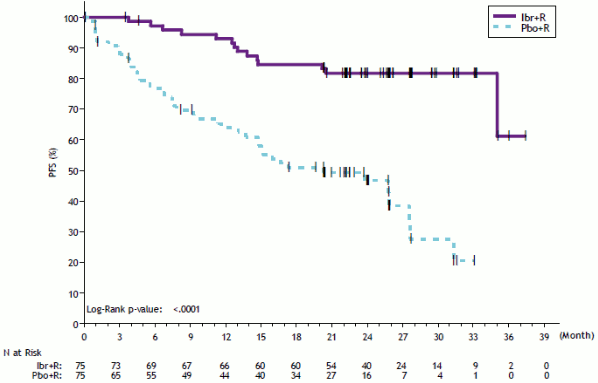
With an overall follow-up of 63 months, efficacy results as assessed by an IRC at the time of the final analysis for PCYC-1127-CA are shown in Table 20 and the Kaplan-Meier curve for PFS is shown in Figure 14. PFS hazard ratios for treatment-naïve patients (0.31 [95% CI (0.14, 0.69)]) and previously treated patients (0.22 [95% CI (0.11, 0.43)]) were consistent with the PFS hazard ratio for the ITT population.
Table 20. Efficacy results in Study PCYC-1127-CA (Final analysis*):
| Endpoint | IMBRUVICA + R N=75 | Placebo + R N=75 |
|---|---|---|
| Progression-Free Survivala,b | ||
| Number of events (%) | 22 (29) | 50 (67) |
| Median (95% CI), months | Not reached | 20.3 (13.0, 27.6) |
| HR (95% CI) | 0.25 (0.15, 0.42) | |
| P-value | <0.0001 | |
| Time to next treatment | ||
| Median (95% CI), months | Not reached | 18.1 (11.1, 33.1) |
| HR (95% CI) | 0.1 (0.05, 0.21) | |
| Best Overall Response (%) | ||
| CR | 1.3 | 1.3 |
| VGPR | 29.3 | 4.0 |
| PR | 45.3 | 25.3 |
| MR | 16.0 | 13.3 |
| Overall Response Ratec (CR, VGPR, PR, MR) (%) | 69 (92.0) | 33 (44.0) |
| Median duration of overall response, months (range) | Not reached (2.7, 58.9+) | 27.6 (1.9, 55.9+) |
| Response Rate (CR, VGPR, PR)c,d (%) | 57 (76.0) | 23 (30.7) |
| Median duration of response, months (range) | Not reached (1.9+, 58.9+) | Not reached (4.6, 49.7+) |
| Rate of Sustained Haemoglobin Improvementc,e (%) | 77.3 | 42.7 |
CI = confidence interval; CR = complete response; HR = hazard ratio; MR = minor response; PR = partial response; R = Rituximab; VGPR = very good partial response
* Median follow-up time on study = 49.7 months.
a IRC evaluated.
b 4-year PFS estimates were 70.6% [95% CI (58.1, 80.0)] in the IMBRUVICA + R arm versus 25.3% [95% CI (15.3, 36.6)] in the placebo + R arm.
c p-value associated with response rate was <0.0001.
d Response rate was 76% vs 41% in treatment-naïve patients and 76% vs 22% in previously treated patients for the IMBRUVICA + R arm vs the placebo + R arm, respectively.
e Defined as increase of ≥2 g/dL over baseline regardless of baseline value, or an increase to >11 g/dL with a ≥0.5 g/dL improvement if baseline was ≤11 g/dL
Figure 14. Kaplan-Meier Curve of PFS (ITT Population) in Study PCYC-1127-CA:
Study PCYC-1127-CA had a separate monotherapy arm of 31 patients with previously treated WM who failed prior rituximab-containing therapy and received single agent IMBRUVICA. The median age was 67 years (range, 47 to 90 years). Eighty-one percent of patients had a baseline ECOG performance status of 0 or 1, and 19% had a baseline ECOG performance status of 2. The median number of prior treatments was 4 (range, 1 to 7 treatments). With an overall follow-up of 61 months, the response rate observed in Study PCYC-1127-CA monotherapy arm per IRC assessment was 77% (0% CR, 29% VGPR, 48% PR). The median duration of response was 33 months (range, 2.4 to 60.2+ months). The overall response rate per IRC observed in the monotherapy arm was 87% (0% CR, 29% VGPR, 48% PR, 10% MR). The median duration of overall response was 39 months (range, 2.07 to 60.2+ months).
Paediatric population
The safety, efficacy, and pharmacokinetics of IMBRUVICA in paediatric and young adult patients with relapsed or refractory mature B-cell non-Hodgkin lymphoma were evaluated in a two-part, multi-centre, open-label Phase 3 study (LYM3003) of IMBRUVICA in combination with either a rituximab, ifosfamide, carboplatin, etoposide and dexamethasone (RICE) regimen or a rituximab, vincristine, ifosfamide, carboplatin, idarubicin, and dexamethasone (RVICI) regimen, as background therapy.
Part 1 of the study (21 patients aged 3 to 17 years) evaluated the dose to be used in part 2 (51 patients aged 3 to 19 years) (see section 5.2).
In part 2, patients were randomised 2:1 to receive either IMBRUVICA as 440 mg/m² daily (age below 12 years) or 329 mg/m² (age 12 years and older) with background therapy, or background therapy alone until completion of 3 cycles of therapy, transplantation, disease progression or unacceptable toxicity. The primary endpoint of event-free survival (EFS) superiority was not met suggesting no additional benefit from adding ibrutinib to RICE or RVICI (see section 4.2).
Pharmacokinetic properties
Absorption
Ibrutinib is rapidly absorbed after oral administration with a median Tmax of 1 to 2 hours. Absolute bioavailability in fasted condition (n=8) was 2.9% (90% CI = 2.1 – 3.9) and doubled when combined with a meal. Pharmacokinetics of ibrutinib does not significantly differ in patients with different B-cell malignancies. Ibrutinib exposure increases with doses up to 840 mg. The steady state AUC observed in patients at 560 mg is (mean ± standard deviation) 953 ± 705 ng h/mL. Administration of ibrutinib in fasted condition resulted in approximately 60% of exposure (AUClast) as compared to either 30 minutes before, 30 minutes after (fed condition) or 2 hours after a high fat breakfast.
Ibrutinib has a pH dependent solubility, with lower solubility at higher pH. In fasted healthy subjects administered a single 560 mg dose of ibrutinib after taking omeprazole at 40 mg once daily for 5 days, compared to ibrutinib alone, geometric mean ratios (90% CI) were 83% (68-102%), 92% (78-110%), and 38% (26-53%) for AUC0-24, AUClast, and Cmax, respectively.
Distribution
Reversible binding of ibrutinib to human plasma protein in vitro was 97.3% with no concentration dependence in the range of 50 to 1 000 ng/mL. The apparent volume of distribution at steady state (Vd,ss/F) was approximately 10 000 L.
Metabolism
Ibrutinib is metabolised primarily by CYP3A4 to produce a dihydrodiol metabolite with an inhibitory activity towards BTK approximately 15 times lower than that of ibrutinib. Involvement of CYP2D6 in the metabolism of ibrutinib appears to be minimal.
Therefore, no precautions are necessary in patients with different CYP2D6 genotypes.
Elimination
Apparent clearance (CL/F) is approximately 1 000 L/h. The half-life of ibrutinib is 4 to 13 hours. After a single oral administration of radiolabeled [14C]-ibrutinib in healthy subjects, approximately 90% of radioactivity was excreted within 168 hours, with the majority (80%) excreted in the faeces and <10% accounted for in urine. Unchanged ibrutinib accounted for approximately 1% of the radiolabeled excretion product in faeces and none in urine.
Special populations
Elderly
Population pharmacokinetics indicated that age does not significantly influence ibrutinib clearance from the circulation.
Paediatric population
Pharmacokinetic data show that ibrutinib exposures in children with relapsed or refractory mature B-cell non-Hodgkin lymphoma, aged 12 years and older receiving a daily dose of 329 mg/m² and those aged 3 years to below 12 years receiving a daily dose of 440 mg/m², were generally within the range of exposures observed in adult patients administered a daily dose of 560 mg.
Gender
Population pharmacokinetics data indicated that gender does not significantly influence ibrutinib clearance from the circulation.
Race
There are insufficient data to evaluate the potential effect of race on ibrutinib pharmacokinetics.
Body weight
Population pharmacokinetics data indicated that body weight (range: 41-146 kg; mean [SD]: 83 [19 kg]) had a negligible effect on ibrutinib clearance.
Renal impairment
Ibrutinib has minimal renal clearance; urinary excretion of metabolites is <10% of the dose. No specific studies have been conducted to date in subjects with impaired renal function. There are no data in patients with severe renal impairment or patients on dialysis (see section 4.2).
Hepatic impairment
Ibrutinib is metabolised in the liver. A hepatic impairment trial was performed in non-cancer subjects administered a single dose of 140 mg of medicinal product under fasting conditions. The effect of impaired liver function varied substantially between individuals, but on average a 2.7-, 8.2-, and 9.8-fold increase in ibrutinib exposure (AUClast) was observed in subjects with mild (n=6, Child-Pugh class A), moderate (n=10, Child-Pugh class B) and severe (n=8, Child-Pugh class C) hepatic impairment, respectively. The free fraction of ibrutinib also increased with degree of impairment, with 3.0, 3.8 and 4.8% in subjects with mild, moderate and severe liver impairment, respectively, compared to 3.3% in plasma from matched healthy controls within this study. The corresponding increase in unbound ibrutinib exposure (AUCunbound,last) is estimated to be 4.1-, 9.8-, and 13-fold in subjects with mild, moderate, and severe hepatic impairment, respectively (see section 4.2).
Co-administration with transport substrates/inhibitors
In vitro studies indicated that ibrutinib is not a substrate of P-gp, nor other major transporters, except OCT2. The dihydrodiol metabolite and other metabolites are P-gp substrates. Ibrutinib is an in vitro inhibitor of P-gp and BCRP (see section 4.5).
Preclinical safety data
The following adverse effects were seen in studies of 13-weeks duration in rats and dogs. Ibrutinib was found to induce gastrointestinal effects (soft faeces/diarrhoea and/or inflammation) and lymphoid depletion in rats and dogs with a No Observed Adverse Effect Level (NOAEL) of 30 mg/kg/day in both species. Based on mean exposure (AUC) at the 560 mg/day clinical dose, AUC ratios were 2.6 and 21 at the NOAEL in male and female rats, and 0.4 and 1.8 at the NOAEL in male and female dogs, respectively. Lowest Observed Effect Level (LOEL) (60 mg/kg/day) margins in the dog are 3.6-fold (males) and 2.3-fold (females). In rats, moderate pancreatic acinar cell atrophy (considered adverse) was observed at doses of ≥100 mg/kg in male rats (AUC exposure margin of 2.6-fold) and not observed in females at doses up to 300 mg/kg/day (AUC exposure margin of 21.3-fold). Mildly decreased trabecular and cortical bone was seen in female rats administered ≥100 mg/kg/day (AUC exposure margin of 20.3-fold). All gastrointestinal, lymphoid and bone findings recovered following recovery periods of 6-13 weeks. Pancreatic findings partially recovered during comparable reversal periods.
Juvenile toxicity studies have not been conducted.
Carcinogenicity/genotoxicity
Ibrutinib was not carcinogenic in a 6-month study in the transgenic (Tg.rasH2) mouse at oral doses up to 2 000 mg/kg/day with an exposure margin of approximately 23 (males) to 37 (females) times the human AUC of ibrutinib at a dose of 560 mg daily. Ibrutinib has no genotoxic properties when tested in bacteria, mammalian cells or in mice.
Reproductive toxicity
In pregnant rats, ibrutinib at a dose of 80 mg/kg/day was associated with increased post-implantation loss and increased visceral (heart and major vessels) malformations and skeletal variations with an exposure margin 14 times the AUC found in patients at a daily dose of 560 mg. At a dose of ≥40 mg/kg/day, ibrutinib was associated with decreased foetal weights (AUC ratio of ≥5.6 as compared to daily dose of 560 mg in patients). Consequently the foetal NOAEL was 10 mg/kg/day (approximately 1.3 times the AUC of ibrutinib at a dose of 560 mg daily) (see section 4.6).
In pregnant rabbits, ibrutinib at a dose of 15 mg/kg/day or greater was associated with skeletal malformations (fused sternebrae) and ibrutinib at a dose of 45 mg/kg/day was associated with increased post-implantation loss. Ibrutinib caused malformations in rabbits at a dose of 15 mg/kg/day (approximately 2.0 times the exposure (AUC) in patients with MCL administered ibrutinib 560 mg daily and 2.8 times the exposure in patients with CLL or WM receiving ibrutinib dose 420 mg per day). Consequently the foetal NOAEL was 5 mg/kg/day (approximately 0.7 times the AUC of ibrutinib at a dose of 560 mg daily) (see section 4.6).
Fertility
No effects on fertility or reproductive capacities were observed in male or female rats up to the maximum dose tested, 100 mg/kg/day (HED 16 mg/kg/day).
© All content on this website, including data entry, data processing, decision support tools, "RxReasoner" logo and graphics, is the intellectual property of RxReasoner and is protected by copyright laws. Unauthorized reproduction or distribution of any part of this content without explicit written permission from RxReasoner is strictly prohibited. Any third-party content used on this site is acknowledged and utilized under fair use principles.